An ongoing dialogue on HIV/AIDS, infectious diseases,
February 15th, 2015
Should Antibiotics be Part of End-of-Life Care?
There’s been some truly outstanding work done recently on end-of-life care, and how we deal with it — or more accurately, how we typically don’t deal with it until the very last moment, at which time often many unfortunate decisions and events occur. Here are three I can strongly recommend:
- Roz Chast’s Can’t We Talk About Something More Pleasant? is probably the most widely read book among my circle of friends right now, as many of us have parents of a certain age. Chast is a cartoonist best known for her distinctive squiggly cartoons in the The New Yorker — here’s one of my favorites — and is already familiar to many ID doctors because of her morbid fascination with dreadful diseases, some of them infections. But this extended memoir about her aging parents is a remarkably ambitious book, by turns funny (of course), moving, and ultimately heartbreaking, especially when touching on the fraught relationship she had with her mother.
- If drawings aren’t your thing, then give Atul Gawande’s Being Mortal a shot. In his usual clear prose — which miraculously reads neither overly technical to the lay public or overly simple to health care providers — he deftly lays out what many of the challenges are in the care of both the elderly and the terminally ill. For example, how can we negotiate the conflict between personal freedom versus safety in our loved ones who have such a limited time to live? If 90-year-old Uncle Milton with severe congestive heart failure wants to eat pickles, but pickles contain too much salt for his diet, should we stop him? The recent Frontline about Atul (we’re on a first name basis, brush with greatness) and his book make me hope that his sensible voice will lead to progress in this difficult part of health care.
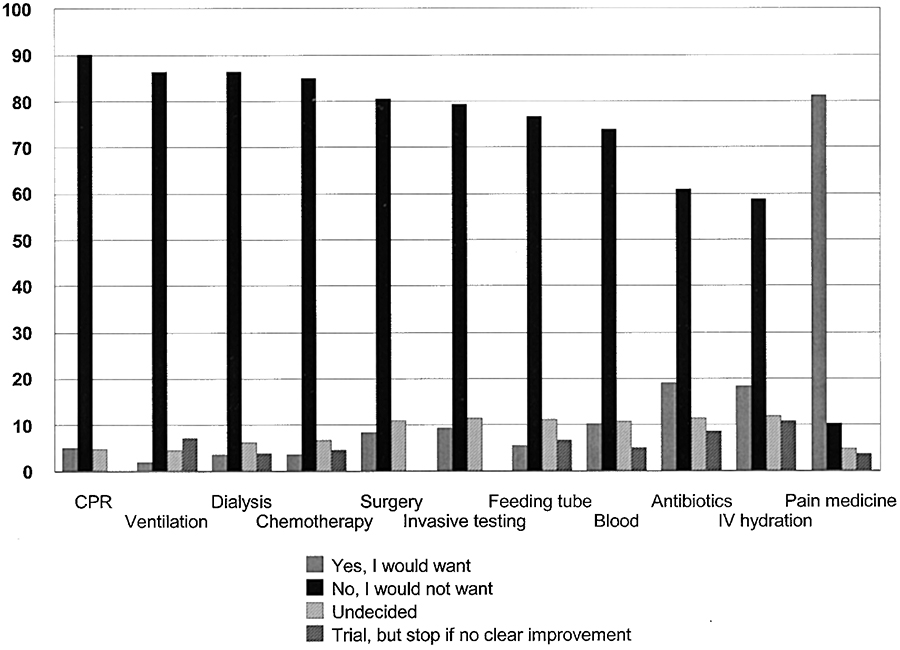
- Finally, if you’re looking for a terrific podcast, check out this Radiolab piece called Dead Reckoning. The first part is about surviving rabies — good stuff for ID doctors, and yes, we’re that bizarre — but the piece finishes in more familiar territory, dealing with medical options at the end of life. In a section called “The Bitter End”, it cites a now famous study done of Hopkins med school graduates, demonstrating that doctors say they would forego end-of-life treatments if they had an incurable brain disease (something akin to dementia) — a big contrast with the people interviewed on the street, most of whom want all this stuff. The end-of-life treatments these doctors considered are shown in the figure below:
Note the ninth one on this list — antibiotics — and consider a scenario that no doubt will be familiar to doctors and nurses the world over, and not just to ID doctors: The patient who has metastatic cancer, or advanced dementia, or irreversible advanced heart or lung disease, and the decision has been made to withhold CPR, mechanical ventilation, tube feeding, and dialysis.
But antibiotics? They often remain an option to the very end, frequently in the face of other conditions with terrible prognoses and little chance for reversal. Those recurrent urinary tract infections, aspiration pneumonias, infected pressure sores, and other indignities of our failing bodies can be treated with antibiotics (though with progressively less effect) — but to what end?
So read the case, take the poll, then listen to the Radiolab piece.
A 94-year-old woman with advanced dementia is referred to the hospital from her nursing home because of fever and a change in mental status. At baseline, she can sit in a chair but cannot walk, feed, or bathe herself; she can respond to simple questions, but has little spontaneous speech. She has an existing DNR order — no CPR or intubation. There have been two admissions to the hospital over the past six months (pneumonia, urinary tract infection), after which she returned to the nursing home. In the emergency room, her evaluation is notable for a fever and somnolence. The urinalysis shows 50-100 WBC. The health care proxy, who lives in another state, is unavailable.


There should be an option c- oral antibiotics, no hospital admission.
If the patient is being transferred to hospital then it should be assumed that she and her family would want full active medical care (besides resuscitation) which would include antibiotics. If on the other hand her dementia is so advanced that she should be palliated, why is she being transferred to the hospital in the first place?
Excellent post. A class that spawned my interest in ID during med school was taught by an old time German microbiologist who said pneumococcal pneumonia was the old man’s friend, and not a bad way to go at the end, as we all gotta go. He was avoiding the (then relatively new) vaccine as he was well past retirement age and teaching for fun.
When my dad was in a NH with late vascular dementia and NPH (DNR, do not hospitalize at his advance directives, he was DMD and ENT MD) they gave him oral antibiotics without my knowledge for pneumonia (my mom could not say no and I found out after the fact; I would have talked her out of it). He recovered to live some more horrible months, when he finally died of strokes in his sleep. Interestingly they had stopped all his other meds like Coumadin for AF, and others in an interest of QOL and to not prolong a life where he did not recognize us anymore, but still gave the darn abx. Annoyed me no end! On many occasions in the hospital I’ve told families Abx were not necessary and could be stopped if they did not want them. Always appalled that as the consultant I’m doing that, but there you have it.
This is one of the Gray area nylon medicine which I suppose all know that is wrong but we still keep doing everyday as we physician’ s are the smartest and at the same time dumbest people in society. We always need someone to tell us that it is wrong. Besides that we should include this important part in the code status itself, like no hospitalization and all the nursing staff and family should be aware of it. The hospitalization should be a part of code status itself. Second think these are the people who have the most resistant infections due to polymicrobial therapy and frequent hospitalization. Great post. Thanks. Needs a dare to bring this up. Surgeon can refuse a surgery if its futile but medicine people can not do that as its just medicine.
Antibiotic stewardship has an important role in this situation as well. I suspect a significant number of physicians may consider antibiotics in end-of-life care futile. Most other futile interventions have an effect only on the patient (and family, payer, care team). But the common practice of treatment with antibiotics at the end of life increases the probability of the emergence of antibiotic resistance, which potentially afflicts the whole community.
http://archinte.jamanetwork.com/article.aspx?articleid=1897550
The wording of those two choices- and making them the only choices- creates a fallacy.
My answer is “Yes, bc to allow a patient to go into septic shock could be next to torture. I’d chose euthanasia over septic shock.”
This article could be included here with all propriety:
http://www.theatlantic.com/features/archive/2014/09/why-i-hope-to-die-at-75/379329/
I think it sums up the feelings of doctors fairly well. I’m considering the topic personally, at 65.
I agree with Pseudonym – it’s not a either or question. In some cases giving an antibiotic could fall under palliative care dependent on many factors including the diagnosis that led to the DNR, the diagnosis that led to considering antibiotics, the age and general health of the individual, etc.
The major downside of treating a terminal patient with antibiotics, is that treatment success also ensures that there will be another cause of mortality inevitably. The benefit of prolonging life in this case, has to be weighed against the potentially horrible ‘benefit’ of more suffering, and possibly a prolonged or painful death from another cause. This needs to be a shared decision, but there is no evil in letting a suffering patient die a comfortable death from an untreated infectious disease (if their wish is to be allowed to die without suffering further). This is an individual and group decision that cannot be made without consideration of all the potential endings – I know having watched many times that death from pneumonia, without IV fluids or antibiotics – can be seemingly pain free and peaceful.
Early involvement of palliative teams, open discussion of futility and assurance of symptom control are the solutions to end-of-life care.
Since this patient has all ready had 2 admissions in the past 6 months for infections, why hasn’t this situation been discussed with her health care proxy because another episode like this is inevitable and we should be focused on goals of care. Hopefully, then she could have a POLST form where she would be DNR/ Comfort Focused Measures Only and would not be transferred to the ER. She could be given oral or even parental antibiotics (IV or IM) at her SNF and be kept comfortable. If she responds, to treatmen, ok. If good comfort care is provided, this is hardly torture.
When my step-father was dying of complications of advanced colon cancer, I insisted that he be given massive doses of pain medication and no antibiotics. We all agreed that his clinical signs indicated that his colon was no longer intact and was leaking into the peritoneal cavity, which was causing a raging infection. There was no efficacious treatment. A family member stayed with him at all times to notify nursing personnel if he gave any sign of pain. The process took 2 days. I believe it would have gone on days longer with antibiotic treatment, creating pointless pain and huge expense with no possible benefit.
If we stick to the case, DNR/DNI does not equal to “no treatment/intervention”. It simply means – do not resuscitate or do not intubate when heart stop beating or no breathing. It is a fairly common misconception among physicians actually. If we closely look at the DNR/DNI order, it does mention that execute the DNR order if there is a terminal illness or a disease with no chance of recovery, Based on that, we have to ask ourself if UTI or pneumonia is a terminal illness. If not, go ahead and treat now and reassess in a few days. Then, provide care withdrawal advice if the infection is out of control with appropriate theray, such as multi-organ failure.
We have heard several stories from the patient’s relatives that they do not want DNR/DNI because physicians become less aggressive in management on patients with DNR/DNI.
We also heard from our colleagues that “oh, this patient is DNR, please don’t overdo.” although the issue would be fixed with a simple test.
Let’s twist the case a bit – if a 35-yo female with advanced multiple sclerosis admitted from the nursing home with the same clinical presentations, what we would do on this patient.
decisions made in end of life care strongly depends on situation. In such case senario where lady is admitted from nursing home and has a short history of illness and acute deterioration in her baseline status. the decision of not for CPR and not for ventilator by no means is an order of euthanasia or support death decision.
If before this illness she was up and around and not dependent on others to me she has all rights to receive appropriate treatment and help to go back to her previous independent state short of those treatment modalities which were already decided and communicated to hospital.