An ongoing dialogue on HIV/AIDS, infectious diseases,
May 29th, 2017
Healthcare Providers Shouldn’t Come to Work While Sick, but They Do — Here’s Why
Let’s start with two questions:
- Have you ever seen a doctor, nurse, PA, pharmacist or other person directly involved in patient care wearing a surgical mask because they have a respiratory tract infection?
- Has this mask-wearing person ever been you?
Bold prediction: Virtually every reader who works in a hospital or large office practice answered “Yes” to #1. Some of you might even have said “Yes” to #2.
Clearly healthcare providers do go to work while sick, and the mask-wearing is our way of saying, “I care.”
But if we really cared, shouldn’t we just stay home?
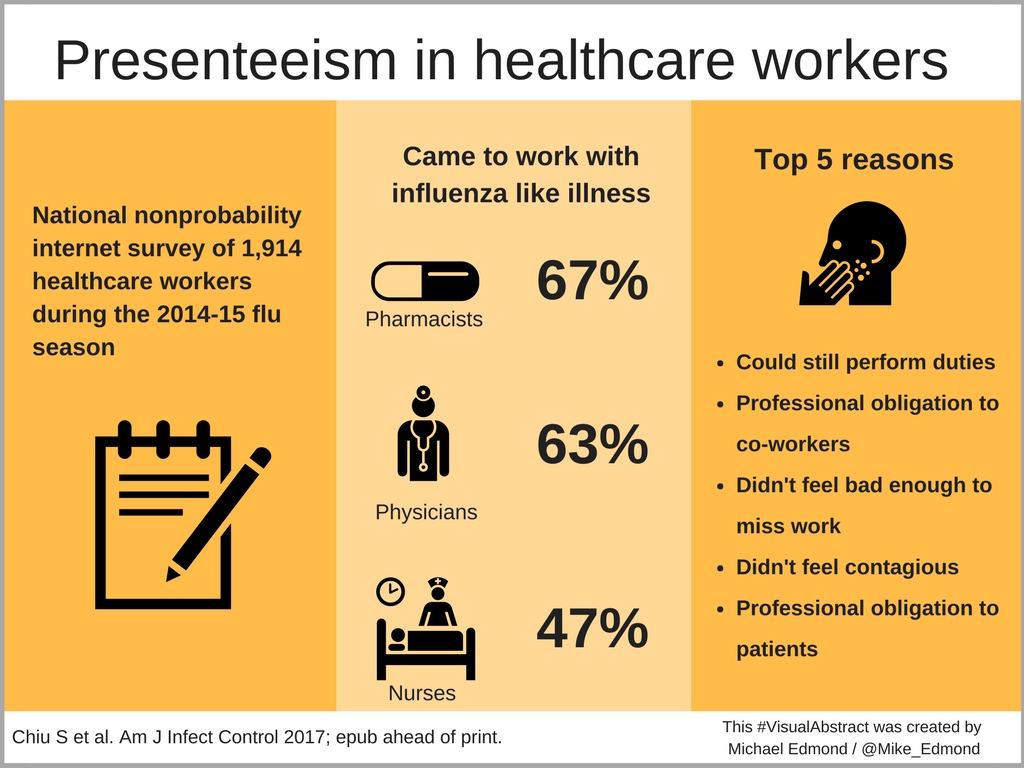
Of course we should stay home. But we don’t. Here’s a recent paper on the topic highlighted by Mike Edmond on his excellent blog, using the nifty “visual abstract” method to present the results:
Remember, surveys aren’t exactly perfect in eliciting whether people are doing some ill-advised behavior. People lie, even in anonymous polls. I know, shocking.
So consider the above estimates of this “presenteeism” a minimum. Yikes. That’s a lot of sniffling, coughing, and potentially mask-wearing healthcare providers out there.
So let’s examine the top 5 reasons why people got to work with an influenza-like illness in a bit more detail; I’ll play the part of the person choosing each response:
- Could still perform duties. Hey, does having a cold preclude me from typing and clicking boxes? That’s mostly what I get paid to do these days, right?
- Professional obligation to co-workers. Who else will do my work? And how can I ask for coverage for what might be “just a cold”?
- Didn’t feel bad enough to miss work. I told you I could type.
- Didn’t feel contagious. If I work while having a cold, I promise to double-down on the hand hygiene — you can call me “Dr. Purell” — and (though it’s embarrassing) to wear a mask. And no one really knows how long a cold is contagious. Symptoms can easily last 1-2 weeks, should I be out the entire time? Impossible.
- Professional obligation to patients. My patients will be mad if I don’t show up. They would prefer to see a sniffly, red-eyed, coughing me than a covering clinician, or to wait a week until I’ve recovered. And obviously no one can provide the brilliant, compassionate, and efficient care that I do.
Jokes aside, presenteeism gives infection control practitioners a major challenge. It’s even more intractable when you factor in the most common reason cited by healthcare providers at long-term care facilities, which is the inability to afford lost pay.
One practical problem we could work on is directly related to reason #4, “Didn’t feel contagious.”
While it’s intuitively obvious that a healthcare worker with pulmonary tuberculosis, active salmonellosis, or highly symptomatic influenza shouldn’t be working, what about milder illnesses that can, in certain hosts, be life-threatening? Thinking about you, RSV, adenovirus, and parainfluenza virus.
Perhaps it’s time we all got a multiplex PCR machine for home use. It would look great in the living room.
Save



Excellent point – perhaps ALL HCP’s should be offered a “Attendance Risk Assessment” – risk of error (dehydration, intoxication, sleep deprivation, etc), stress (in and out of the job), risk of acquiring an infection (needle stick etc.), risk of infecting someone, and that the Agency would say below X points you are paid to not take the risk (“sick days”). Not uncommon for people to be far more impaired by divorce than RSV.
The second part of point 4 is critical. Influenza can last 7-10 days, as can many common colds. To stay out for the duration of the illness would put considerable strain on the healthcare system you’re working in, especially when other HCPs are likely to have the same thing at the same time. I’m not sure what the answer is, but simply staying away from work whenever you feel bad clearly isn’t it.
The criticality of this message is not to be sneezed at (pun intended.)
We have structured a system that makes this occurrence predictable.
In EM, we are scheduled in such a way that you have to have a signed death certificate AND a note from your mother to be absent.
Given no administrative plan for backup in the event of illness coupled with a lack of sick days that you’re expected to take, it seems to me that the system is getting exactly the results it set out to achieve!
Tom you are spot on with your comments- I do agree!!!!
The system fails you when you are ill. In many ways management does not care… only if their quotas are met!
One even gets the 3rd degree on their return to work on why you were not here!
#2 and 5 are huge. As a Hospitalist, I can’t just cancel my clinic. If I don’t come in to work, patients don’t get taken care of. We are short staffed as it is, with no real back up plan for sick days. Unless I’m admitted to the hospital, I’m going to show up for work. If there is a serious illness, it will be very difficult to get cross coverage, but necessary. If a less serious illness, I just will have to work through it. What’s wrong with using a respiratory mask anyway?
Unless there is a backup plan created or there’s some reason to think good hand hygiene and use of respiratory precautions doesn’t work, I will work. Besides, if respiratory precautions don’t work, why are we depending on them to prevent transmission from our patients to us in the hospital?
I should say that I would not work if illness was significant enough to make me unable to work or if there was not a good way to prevent transmission. For a mild respiratory illness, this would not apply.
I would add “tried to get care but couldn’t” to why we work sick. I tried to do an eVisit for a sinus infection during my own block of back to back 12-hour shifts. The software kicked me out as ineligible because of my age (66) and recommended I go to an Urgent Care or ER. This despite the system having access to my medical records which could demonstrate my good health, no chronic medical conditions, and no prescription medications. Sure, I suppose I could have gone to the ER after my shift was over and waited a few hours to be seen for a problem that did not merit the acuity level of an ER visit or of my ER colleagues’ time. But wouldn’t it make more sense to actually use the electronic records like they should be (to get a picture of the patients’ health), and/or adjust the algorithm for eVisits?
Providers have the same kinds of access issues as our patients do, or at least us “seasoned” providers do. I have no illusions about my employers’ ability to carry on its business without me – I would just prefer not to drop dead at work!
I strongly advocate for a “Medical Professional OSHA”. While many entities claim the validity of their existence by striving for patient safety, physical & mental health of providers, and risk management, none of them pursue the basic rights of any workplace environment. Now with bIG cORPORATE involved, policy makers might consider putting some teeth into basic protections. A related issue is making our profession millennial friendly. Lastly, if you don’t take care of the work force, the work force won’t be in a position to take care of you……
Stop whining and go to work.
I am among those who go in when sick, unless it is a GI bug.
I HATED being home after my ACL transplant; it was less than 7 days, but I felt like I was getting so behind (that was in 2010….)
I will try to do better. But all I really do is type and check boxes.
Sometimes I feel that it is a matter of pride as well for some Health Care Professionals.
Med Techs notoriously have a higher lymph count from ongoing exposure, but give me the mandated flu-shot and I’m out for 5 days. Messes with my otherwise strong immunity.
Well why is there not a reason “not enough sick days provided”? I come to work sick because I have two little kids and ONLY 5 sick days in a year. And IF I call out sick more than 2 times in3 months I get written up! I get a disciplinary action. And it’s all absolutely legal here in the US. They don’t care apparently if I’m sick or not, they just want me to foloow their rules.
SO I only call out for my kids. No hours left for me! There’s no social safety net inthe United States and that’s why people come sick to work in general and in healthcare as well.
Hi!: you’ll be surprised, reading about histories of men and women considered models of life, blessed or saints, how many, knowing they had Tuberculosis, but in pre-antibiotic era, continued their stay in an environment with presence of kids or susceptible persons, as teaching, care,…
Also, some cases of contagion from diseases as Actinomycosis from extreme behavior, as kissing ulcers of patients under care, seem existed. The most bizarre case was a monk in a cloister, considered saint, who received every night the visit of a woman in his cell’s bed, had sex, with the woman disappearing in the morning, same ignored way as she came in (Through the bathroom window?). Regards, + Salut
I worked in a for profit hospital pharmacy. I didn’t miss a single shift in 3 years. One winter day, I called in sick – fever/headache/bad body aches, the whole 9 yards. My shift that day would include rounding on the oncology unit. I was fired for absenteeism. Per hospital policy, employees were required to give notice of illness the day prior to the sick day. I’ve since moved on but still reflect on the poor judgements of my old, continually understaffed pharmacy. Focusing on the bottom line meant it was the norm to come to work sick and contagious. It would be interesting to assess hospital acquired illness rates/numbers by type of hospital (community, academic, for profit, non-profit).
How about this: I am required by my facility’s policy to not come to work for seven days after onset of flu symptoms. So policy literally states I am not allowed to work, but then goes on to state “attendance policy fully applies”. In effect, I would get punished, and in order to get paid I have to use my earned PTO, because I am not allowed to go to work. Only in the USA.
I think there is need for an objective assessment of the conditions before determining if or not to skip work and for how long….. May be if there risks of transmitting to all the rest plus your clients then keep off…