An ongoing dialogue on HIV/AIDS, infectious diseases,
November 18th, 2015
Are There Remaining Challenges in HCV Therapy?
Prompted by (yet more) spectacular HCV study results, I posted the following questions on Twitter:
Is velpatasvir/sofosbuvir the endgame for HCV? And what will HCV researchers do now? https://t.co/vL2A9FOttR @NEJM
— Paul Sax (@PaulSaxMD) November 18, 2015
To which I got this reply from one of our very energetic second-year ID fellows:
@PaulSaxMD @NEJM what about coinfected patients, drug interactions?
— Philip Lederer (@philiplederer) November 18, 2015
OK, OK, I know what you’re wondering — don’t you two have anything better to do than fool around with a financially struggling social media platform?
Sure we do — but after years and years of “not getting” Twitter, I now (thanks to Phil) see some of the benefits, namely the rapid exchange of information and ideas, in a particularly efficient form.
But back to the topic at hand, which is the HCV regimen used in these latest studies published in the New England Journal of Medicine. All include the pan-genotypic NS5A inhibitor velpatasvir with the already-approved nucleotide sofosbuvir, given as a single pill once daily.
Results? Outstanding:
- Genotypes 1, 2, 4, 5, and 6: 99% cure.
- Genotypes 2 and 3: 99% and 95% cure, respectively.
- Decompensated cirrhosis: 86-94%.
The results really make you wonder what more we can do to make HCV treatment better. We are definitely at the flat part of the 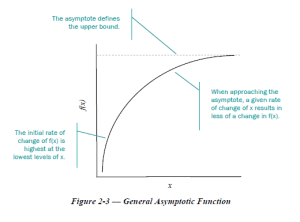 response curve, and fortunately it has plateaued way up there, with 95% or higher cure rates for all but the sickest HCV patients, along with exceedingly rare adverse effects.
response curve, and fortunately it has plateaued way up there, with 95% or higher cure rates for all but the sickest HCV patients, along with exceedingly rare adverse effects.
So are there remaining issues? Yes, sort of — but none of them is as pressing as the obligatory elephants in the room, which are cost and access. Let’s start with Phil’s proposed challenges, plus a few others:
- Co-infected patients. Not really a problem at all — people with HIV respond just as well as those without coinfection. (Several examples of studies cited in this post.) In fact, in many ways they’ve been easier to treat, as the patients are already used to taking medications every day.
- Drug-drug interactions. Compared to what we’ve dealt with using ritonavir and cobicistat and rifampin, these are a piece of cake — unless you’re actually using ritonavir with the “PrOD” regimen. (That’s what I’ve been calling it. I never liked “3D”.)
- Cirrhosis. Especially with a history of treatment failure to interferon-based therapies. In most studies, the newer drugs don’t work quite as well in these patients — but we’re generally talking small differences. Response rates are still pretty great.
- Patients who have failed treatment with an NS5A inhibitor-containing regimen. Indeed, this does limit our options quite a bit, and assessing for resistance is anything but straightforward, especially with non genotype 1. But we’re not completely without options — alternative sofosbuvir-based regimens will work in some patients, as the resistance barrier to this particular drug is sky high. I suspect we’ll get some clarity on this issue over the next several months.
- Patients who can’t take 12 weeks of therapy. Most studies of treatment for less than 12 weeks have been disappointing. Does a shorter course mean better adherence? Lower cost? Better outcomes? Maybe. Hard to beat the current rate of cure, but still — a regimen that could be given for 2-4 weeks would be welcome for some patients. Think H pylori treatment, if you can stand the analogy, since ID doctors know squat about H pylori therapy.
- Cost. See elephants in the room, cited above. Maybe the soon-to-be-approved grazoprevir/elbasvir. We’ll see.
So what about the second part of that tweet?
And what will HCV researchers do now?
I don’t know — become experts in implementation research? Study how to cure hepatitis B? Switch to steatohepatitis? Fibrosis reversal? Learn how to juggle clubs?
[youtube http://www.youtube.com/watch?v=Ax0wl8pYk4g&w=560&h=315]


How about testing – rapid RNA test? And pregnant women – need to prevent MTCT. And a long-acting formulation would help with adherence issues (one time injection?) And of course, the elephant, how do we get these amazing meds to the people who need them when we are faced with high costs and unscientific restrictions from payers? Still more work to be done.
How about a Hep C vaccine? And like Sarah, I was also thinking about pregnant women.
Interesting thought. But if you have a disease that targets only at-risk individuals and is all but 100% curable, one could argue that a vaccine isn’t really going to be widely deployed, or that useful. There’s been a bit of an increase in HCV along with the rise in injection drug use in this country, but the incidence dramatically declined with the screening of the blood supply which started in the early 1990s.
Paul
What can we do now?
The HCV community needs to make connections with the addiction/ harm reduction communities.
Stigma against people who use drugs is enormous. This is a political/public health problem.
We can take the lead.
What about the scope of treatment in renal transplant pt with hcv regarding side effects , risk of rejection , to treat or not ?
Regarding remaining challenges in HCV therapy:
If the current nucleotide inhibitors of NS5B (which are pangenotypic with a high resistance barrier) lose their effectiveness at faster rates due to mutations/changes in HCV’s NS5B active site then we might start relying more on the help of other comparatively “inferior” anti-HCV drugs such as the NS3/4A inhibitors and nonnucleoside NS5B allosteric inhibitors which have a low barrier to resistance and are not pangenotypic. Research to improve these drugs, and other classes still early in the development phase, would be in the public’s interest and would serve as an insurance policy to fall back on.
Recent case reports highlighted reactivation of previously dormant HBV when HCV coinfected patients were treated with the all-oral anti-HCV medications. This issue would need to be addressed since it did not seem to be a complication of the older PEG-IFN+RBV therapy.
I think anti-HCV vaccine would still be required for a few reasons.
* In theory, an anti-HCV vaccine might be capable of preventing hard outcomes more effectively than treatment.
* Vaccines would be expected to be a less expensive alternative to lengthy and expensive drug treatments of chronic HCV infections which may save society untold amounts of precious healthcare dollars.
* By preventing disease in the first place vaccines may prevent suffering and social stigma associated with diseases like chronic HCV infections which in turn may help HCV patients address their underlying mental health issues more effectively.
* In areas of the world where medication coverage is publicly funded (e.g., Canada, many European countries), it might be a bit controversial (rightly or wrongly) when the public is asked to cover expensive anti-HCV medications for a condition that is most commonly contracted due to injection drug use. The probably less expensive vaccine (if it were available) might be the acceptable answer in these economies and might shift resources to other desperate areas in healthcare.
* Although current HCV treatments reduce the viral load to undetectable levels, treated patients may contract HCV again necessitating yet another round of expensive treatment. Anti-HCV vaccines would be expected to eliminate this possibility.
Agree with the HCV reinfection/retreatment problem and possible failure of current drugs due to viral mutations.