An ongoing dialogue on HIV/AIDS, infectious diseases,
June 12th, 2016
Progress in Lyme Disease Badly Needed — Could a “Hackathon” Help?
Someone recently asked what keeps me, a specialist in Infectious Diseases, up at night.
With the admission that I do all my clinical work here in the USA — a person working in the tropics would undoubtedly have a different list — several challenging patient care and public health issues came to mind. Multidrug-resistant bacteria. Endovascular infections in patients with opiate addiction. Surgical infections with poor “source control”, especially in the abdomen. Non-tuberculous mycobacteria. Recurrent C diff and MRSA. Patients who, despite having access to lifesaving HIV therapy, don’t take their meds. An aggressive, transmissible flu strain arising from our close contact with birds or pigs. Aedes albopictus starts transmitting dengue, chikungunya, and Zika. Drug prior approvals that defy medical common sense. Electronic medical records that force docs to become overeducated clerks.
And, of course, Lyme Disease.
I’m far from alone about this concern, by the way. In an effort to make some progress against this challenging infection, a “healthcare hackathon” on Lyme will be held in Cambridge June 17-20, led by the Dean Center for Tick Borne Illness. And if you’re wondering what a healthcare hackathon is, one of the Dean Center’s doctors kindly shared this review — it’s essentially it’s a way of bringing together experts from multiple fields to work together and tackle a problem.
This approach makes abundant sense, as solutions to complex problems rarely come from a single discipline.
And boy, is Lyme the very definition of a complex problem, a keep-you-up-at-night topic — allow me to list why:
- Lyme has become way more common. When I became an
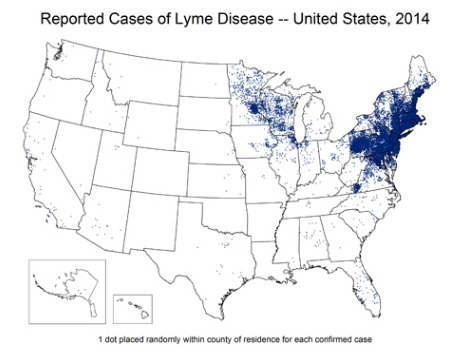
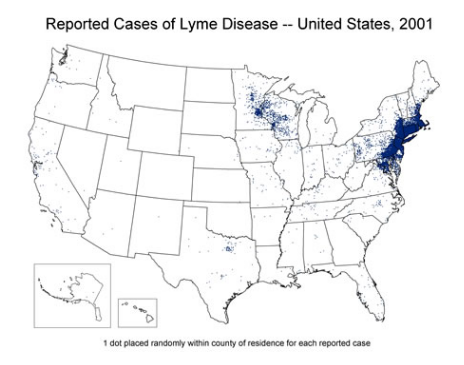 ID specialist in the early 1990s, most of the people we saw with with Lyme lived on or near the coast, or had visited Cape Cod, Nantucket, or Martha’s Vineyard; now we see Lyme acquired throughout New England, and even in urban areas. It is spreading from the Northeast and Midwest into the South, and it no longer disappears completely in the winter — all it takes is a prolonged warm spell, and a few cases pop up. Here are the numbers per CDC — there are 300,000 cases/year in the USA, a substantial increase over the last 3 decades, and no doubt an underestimate since many cases are not reported.
ID specialist in the early 1990s, most of the people we saw with with Lyme lived on or near the coast, or had visited Cape Cod, Nantucket, or Martha’s Vineyard; now we see Lyme acquired throughout New England, and even in urban areas. It is spreading from the Northeast and Midwest into the South, and it no longer disappears completely in the winter — all it takes is a prolonged warm spell, and a few cases pop up. Here are the numbers per CDC — there are 300,000 cases/year in the USA, a substantial increase over the last 3 decades, and no doubt an underestimate since many cases are not reported. - Severe Lyme Disease is a bad problem. Yes, most cases of
 erythema migrans respond promptly to therapy; there are even people with positive tests who have never been treated and feel totally fine. That’s the good news, the mild end of the spectrum. But rarely, especially (in my anecdotal opinion) for those who get sick and delay diagnosis and treatment, Lyme can be very serious — high fevers, cardiac disease, hepatitis, arthritis, encephalitis, meningitis, neuropathies, radiculitis, myelitis. And these severe cases are those most likely to have residual symptoms after treatment.
erythema migrans respond promptly to therapy; there are even people with positive tests who have never been treated and feel totally fine. That’s the good news, the mild end of the spectrum. But rarely, especially (in my anecdotal opinion) for those who get sick and delay diagnosis and treatment, Lyme can be very serious — high fevers, cardiac disease, hepatitis, arthritis, encephalitis, meningitis, neuropathies, radiculitis, myelitis. And these severe cases are those most likely to have residual symptoms after treatment. - There is no proven optimal treatment for patients with ongoing symptoms after Lyme. Some people think it’s best to try more antibiotics, targeting residual active bacteria. Others (read: most ID doctors) think that’s not a good idea, for four main reasons: 1) The scientific data on residual living spirochetes after treatment are far from definitive; 2) Several controlled clinical trials — most recently this one — show no benefit long-term antibiotic therapy; 3) Post-infectious symptoms may occur after many severe infections (bad influenza, sepsis, endocarditis, pneumonia, toxic shock syndrome), and we don’t give long term antimicrobial therapy for these conditions; 4) Antibiotics can be harmful — a colleague of mine notably had a patient who required a colectomy after developing C diff on a prolonged course of ceftriaxone prescribed by a Lyme specialist. Still — if we’re not giving antibiotics, what are we offering? To quote this excellent editorial that accompanied the above cited clinical trial — “Though prolonged antibiotic therapy is not the answer, we do not know what is truly helpful.” (Emphasis mine.) No wonder our patients are unhappy!
- Testing for Lyme is confusing, sometimes inaccurate, and slow. Think how accurate HIV testing has become — sensitivity and specificity are way north of 99%, false-positives and false negatives extremely rare, and generally quite easy to sort out with supplemental tests. HIV test results are back quickly, either right away with a point-of-care test, or at most a few days. Lyme testing is the opposite — early in disease, antibody testing lacks sensitivity; later on, the two-step procedure of screening ELISA followed by Western blot is fraught with false positives (especially IgM immunoblots) and, according to some, false negatives. Delays in receiving definitive results are common, and labs do not all have the same criteria for positivity. Molecular testing with PCR is of limited accuracy (even in acute disease), and follow-up Lyme antibody tests after treatment don’t provide proof of cure. The problems with standard Lyme testing have spawned a variety of “home brew” alternatives — here’s a terrific brief review — and note that none of them is FDA-approved, many require that desperate patients pay out of pocket, and all add to the confusion about who does and who does not have the disease. Thank you very much. (That was sarcasm.)
- Instead of cooperation, there is pervasive rancor in much of the discourse on Lyme. For whatever reason, the difficulty in prevention, diagnosis, and treatment of Lyme has created conflicts between patients, providers, and public health officials — a conflict far different from other challenging diseases. For example, the documentary Under Our Skin repeatedly attacks the medical community for ignoring the disease, and promotes numerous unproven diagnostic tests and treatments. There are several unfortunate results of this conflict, but one of the most discouraging from my perspective is the very speciality that should be front-and-center in trying to solve the problem — Infectious Disease — is repeatedly attacked; under that attack, ID doctors sometimes dig in their their heels on these controversial issues, or ignore them entirely, and the discourse stops. One can read opposing views on this from activists and IDSA here and here, respectively.
This last item (the controversy) is the reason why, for the last several weeks, a green flyer promoting the Lyme Hackathon has been posted in our clinic, and I’ve kept a copy on my desk. Notably absent from the pre-meeting materials are attacks on either side of the debate — a refreshing change from the usual harrangues.
I wish them the best of luck — we are all hoping for some progress!


Most patients who have been diagnosed with chronic lyme disease have been misdiagnosed. In many it is a conversion disorder. Most “lyme disease specialists” severely overcharge their patients and are little more than quack physicians. Specialists who pander to the special needs of quack physicians are no better than the quack.
Paul – compelling and well-balanced presentation (as always) of the significance and challenges of Lyme. Can you comment on a Lyme vaccine? Hasn’t such a vaccine been developed, but shelved due to lack of market opportunity? Doesn’t such an opportunity now exist?
A vaccine was approved in the 1990s, but it was voluntarily withdrawn by the manufacturer due to low sales — likely triggered by the fact that some claimed to develop chronic joint symptoms after getting the vaccine (etiology never proven). Great review here:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2870557/
For the record, it had a clever brand name: “LYMERix”, a la “limericks”.
Paul
Paul- Vaccine did not have poor sales to my knowledge. some people got lyme symptoms from it esp after the booster shot. You state non proven of course.
Dr. Allan Steere said in a conference talk ( after–the vaccine was removed from the market) that anyone who had the DL-4 gene in their blood if they got the vaccine shot they would develop a non retractable arthritis. People should have been tested for the gene before receiving the vaccine- a simple blood test–yet this was not revealed.
Dear Paul,
the battle is also raging here in Europe; a lot of patients with fibromyalgia, chronic fatigue syndrom or others ‘strange’ symptoms (please read the paper: Long-term sequelae of West Nile virus-related illness: a systematic review Hetal Patel et al.
The Lancet Infectious Diseases;Volume 15, Issue 8, Pages 951-959 August 2015) are convinced by other patients, internet and/or ‘physicians-self-proclaimed-specialist -in- Lyme -disease’ that a ‘cold infection’ (with probably other unrecognized co-pathogens such as Babessiosis, Ehrlichiosis, Rhickettsiosis, Chamydia, Bartonella,…) is realy under their skin and are coming to receive prolonged course of antibiotics (in reality, the vast majority of them received several courses of several antibiotics prescribed by their GP before coming in the ID visit).
Here in Belgium, a lot of conferences are organized by activists without objective open debate, inviting ‘stars of Lyme Disease’ coming from USA (it’s still better in USA when your are living in Europe) or from Paris (it’s still better in Paris when you ‘re not living in Paris!),saying that (1) physicians (including ID specialists) cannnot recognize the disease (but they can), (2) usual testing are poor in terms of sensitivity and specificity (but they have the good tests) and (3) current national and international treatment guidelines are inappropriated (but they know how and how long to treat you). It took a lot of time, patience, and convicing power to explain, as you wrote, that ‘though prolonged antibiotic therapy is not the answer, we do not know what is truly helpful’.Thank you very much. (That was sarcasm.)
We have ticks all over Georgia. My son has been infected several times both in Maryland as a teen and here in Georgia a an adult. However, every doctor he saw in Georgia emphatically said there is no Lyme disease in Georgia. He has neurological, cardiac, gastrointestinal and more symptoms. He had to move back to Maryland to receive treatment from a MD specializing in Lyme.
I’m retired now but when I was in ID practice in Milwaukee, I made extensive use maps indicating distribution of Lyme cases, but not the ones showing the patient residences. More useful were the maps showing the places to which they had traveled where they had contracted the infection. The cities of Milwaukee, Minneapolis, and St Paul are not high risk areas.
This may seem like a rather mundane question, but is there any evidence of a significant advance in any field that can clearly trace its origin back to a “hackathon”? I understand the enthusiasm and the theoretical benefit and I suppose the generation of novel ideas is the beginning of any movement, but I’ve yet to see any evidence that any “hackathon” has led to changes / improvements in public health. Take the Ebola “hackathon” for example. All of the progress made in this disease in the past year has been made in more traditional forums of research and development . I am not familiar with other arenas such as development.
I would actually genuinely like to know where have the ‘winning’ ideas gone once a ‘hackathon’ is over? Otherwise it seems like just another networking event, which is probably a positive thing but overall not very unique.
This is a great question. At the hackathon, it was pointed out that from at least the MIT hacking medicine hacks, more than 18 companies have been funded and have raised $90M.
Changes in healthcare diagnosis and treatment come glacially given regulatory structure of the industries. But a hackathon can be an excuse to think of new ideas to apply to an old problem (prize money doesn’t hurt either). And if you fail, well it’s only a weekend.
At this hack, two new therapeutic approaches to borrelia infection were investigated. I dare say the opportunity to work on these in a hack format, with clinicians and scientists to mentor in real time, brought these further along in 3 days than otherwise would have been done in 3 months.
I was skeptical as well, but it turns out it proved to be a great way to jumpstart some ideas in a therapeutic area which is sorely in need of them.
Great idea.
I won’t agree that long-term antibiotics don’t help because they’ve helped me to recover from very serious neurological, heart and brain problems. I’ve seen what antibiotics do to my body first hand and I will be absolutely astonished if persistent infection is not at the center of this problem. All this said, I wonder if resistant strains of Babesia will turn out to have a more important impact on patient symptoms than the persisting Bb infection everyone seems obsessed about. A year of IV antibiotics definitely helped a lot (I had POTS and exhaustion so bad I couldn’t stand up to cook for 5 minutes and pain so bad I nearly committed suicide twice and both responded to treatment starting about 5 months in), but it was Coartem and Mepron that really moved the needle, especially with regard to air hunger, night sweats, fevers and so forth.
Regardless of the considerable disagreement and acrimony, I think we can all agree wholeheartedly that treatment of Bb infections, especially when multiple co-infections are involved, is really terrible right now in terms of efficacy. It’s not an understatement to say that Bb+Babesia+Bartonella has ruined the last 15 years of my life and nearly ended my life last year. There has to be a better way. The suffering caused by this disease is beyond what most physicians can conceive.
Try the Stephen buhner herbal protocol it worked for me I was almost dead too now 95% better
If antibiotics work for you, then why are you still sick?
You’re right that I’m not cured, and I really wish we knew more, but there’s an enormous difference now versus when I was untreated and only getting sicker and sicker. I am able to live my life again, although with some limits. There’s no question in my mind that without treatment I’d simply be dead now. We desperately need research and better treatment for this terrifying illness.
Here’s a link to an in-depth analysis of contested findings and recommendations included in the Infectious Diseases Society of America guidelines for diagnosis and treatment of Lyme disease.
Active Infection: Clinical Definitions and Evidence of Persistence in Lyme Disease
Analysis of 2006 IDSA Guidelines by Steven Phillips, MD
http://www.lymepatientadvocacy.org/Porfolio/AnalysisofIDSAGuidelines.pdf
I contracted undiagnosed Lyme, documented by the CDC to produce Lyme antidotes due to past antibiotic treatments for a sinus infections over the years. CDC has documented Urgent Active Rocky Mountain Spotted Fever, not once but twice while living in Georgia! I have Fibromyalgia, lack off cartilage in joints and chronic fatigue. I don’t produce any IGA or IGE any longer and have had past IGG infusions to boost my worn out immune system. The last RMSF was from one tiny tick that had crawled up under my middle toenail while wearing sandals going between the house and car. I hadn’t been outside during the infectious timeframe for anything else due to another issue. What does that say about the transmission possibilities? My doctor said the CDC commented on the increased number of documented cases of RMSF in Nth. Georgia during the of summer 2012.
Nice to hear my former colleague, Dr. Lauwasser, on these comments. There is certainly a vocal and strong anti-science/conventional medicine organization. I know of people that become enraged with just the mention of the name Dr. Wormser. Unfortunately there are other instances, e.g. the anti-vaxers and autism. Tick borne diseases is a complex problem. I can only hope that someone will have that ah ha moment; or perhaps it’s really a complex answer with multiple solutions. Chronic debilitating disease is no fun (sarcasm and an understatement). It’s hard for both sides to understand the difficulties that they face. It’s easier to blame. Good luck.
In Kenya where i practice Lyme is rare but recently we recorded cases from around the Tana delta area . majority presented with musculoskeletal symptoms with 2 patients presenting with heart block. no patient could recall having had the classic rash.