June 2nd, 2022
The Importance of Psychological Safety
Brandon Temte, DO

Dr. Temte is a Chief Resident in Internal Medicine at Providence Portland Medical Center in Portland, OR.
Even before starting residency, I knew I wanted to be a critical care doctor. I chose my residency program and drove halfway across the country to get a solid hands-on clinical experience. As an intern in the ICU, I was eager to get involved in every possible way. One morning after team rounds, fully caffeinated and ready to call a few consults, I heard the speakers sound, “Code Blue, CCS 9.” I immediately dropped everything and ran to the room. This was the 31-year-old man I had just admitted for a polysubstance overdose.
Deer in the Headlights
As I arrived at the code, I could see my attending standing in the doorway. The nurses started chest compressions, and the usual chaos was all around. Alarms were screaming, and a desperate family was standing outside the door. As I approached the room, my mentor and attending turned to me and said, “Are you ready?” I nodded and took a breath. He turned to the rest of the room and stated loudly, “Alright, everyone, Dr. Temte is running this code!”
 I memorized algorithms and watched numerous codes, but this was my first time as the leader. I assigned roles, gave the first shock, and ordered a dose of epinephrine. My heart was racing out of my chest. My attending turned to me and asked, “What now?” I completely froze. Everything I had learned melted away, and I had no response.
I memorized algorithms and watched numerous codes, but this was my first time as the leader. I assigned roles, gave the first shock, and ordered a dose of epinephrine. My heart was racing out of my chest. My attending turned to me and asked, “What now?” I completely froze. Everything I had learned melted away, and I had no response.
Overwhelmed, I took a step back. I’m sure I was white as a ghost. My attending confidently took back lead of the code until the patient had a pulse. “What on earth just happened?” I muttered to myself.
Success in Failure
Later that same day, my attending found me in the call room. He said something unexpected. “Great work in there!” In a frustrated tone I responded, “I totally failed! I froze after a minute. I thought I was prepared for this.”
 He responded, “Now that you’ve felt the weight of the room, you’ll know what to expect next time. That’s how everyone’s first code goes! Putting yourself out there the first time is the hardest part.”
He responded, “Now that you’ve felt the weight of the room, you’ll know what to expect next time. That’s how everyone’s first code goes! Putting yourself out there the first time is the hardest part.”
This was a pivotal moment in my career, and I learned an important lesson that day: Active learning in a safe environment is key to adult learners becoming excellent clinicians.
We regularly find ourselves in new situations throughout medical school and residency training. However, we also start our early careers in an environment where performance is being constantly evaluated. Fear of appearing incompetent or unprepared can limit the desire to seek novel experiences. At times, we would rather lean back on our comfort zones of a perfect patient presentation or an already well developed clinical framework. Psychological safety is the belief that members of a team have a safe space for interpersonal risk-taking¹. This protected space welcomes learners to push their boundaries and be active participants without fear of negative consequences.
Creating Psychological Safety
Throughout my career as a resident and now an attending, I’ve seen excellent clinical and interpersonal skills develop alongside discomfort. As adult learners, especially in residency, we need to be active participants in the challenges we face. Utilizing a growth mindset requires leaning into the discomfort at times. The first hypotensive patient you take the lead on will inherently be uncomfortable. If done in an area of psychological safety, these early experiences can provide the firsthand experience to acquire excellence.
 That day in the ICU, running my first code, my career took a large step forward. I realized the importance of the support I received. The nurses, senior resident, and attending saw my desire to improve, not the skill gaps I was so self-conscious of displaying.
That day in the ICU, running my first code, my career took a large step forward. I realized the importance of the support I received. The nurses, senior resident, and attending saw my desire to improve, not the skill gaps I was so self-conscious of displaying.
Creating a space with psychological safety requires intention. Preparation prior to the encounter is key to confronting new situations with confidence. Pre-briefing with all members of the team regarding roles and duties can help with learner comfort. To the learners, be clear regarding what you are specifically working on so the other leaders on your team can allow room for growth. To all those about to step into a senior resident or attending role, set the stage early by setting clear expectations. Explicitly call out the safe learning environment.
Medicine is a demanding profession, but we all deserve a safe space for active learning to become excellent physicians.
- Edmondson AC. The fearless organization: Creating psychological safety in the workplace for learning, innovation, and growth. Hoboken, NJ: John Wiley & Sons, 2018.
May 25th, 2022
The Pandemic Through a Rearview Mirror
Abdullah Al-abcha, MD
Throughout medical school, the word pandemic was something distant from our world of advancements. We truly believed we had reached the epitome of a future where a virus is something we could contain. COVID-19 proved us wrong. In March 2020, the World Health Organization (WHO) declared a pandemic. An unprecedented event that would change our world. An epic event that we considered to be something of the past forced us to hurry into a virtual future we all feared. Many people were overworked, others lost their jobs, and too many lost people dear to them.
As healthcare workers, we were affected like everyone else, but it was our role to fight the pandemic — face to face — on a daily basis. As with all unfortunate events, it’s odd to speak about the good side of the COVID-19 pandemic, but it has altered our profession in unconventional ways: Everything from seeing patients virtually in their own homes to attending conferences around the country from the comfort of our couches.
Learning at your convenience
During the first year of the pandemic, I was serving as the junior chief resident. My responsibilities involved arranging our departmental weekly didactics sessions, but everything was different, everything was virtual! Rereading this sentence, it seems normal and insignificant, as we were already headed toward a virtual world (despite everyone’s fears) for many years, so it shouldn’t have been a surprise — but in reality, it was. In addition to life occurring mainly through screens, when we did see people, we had to maintain a distance of 6 feet apart. It felt impossible, given the congestion of the world we were used to living in.
 In 2020, apart from the auditorium, our hospitals had no conference rooms built to host 50 residents while keeping them safely 6 feet apart. So, like everyone else, we needed to arrange our didactics in livestreaming sessions. This seemed limiting, at first. However, these live online sessions expanded our departmental didactics like never before. First, it gave us the opportunity to record all of the sessions, start a YouTube channel, and have all of our recorded lectures available for our on-call residents who missed them and for anyone interested from around the world. Second, we were able to invite speakers from all over the country, including our previous graduates. Third, residents were able to join our live sessions from our main training hospital, off-campus clinics, and their own homes (which increased our residents’ attendance rates). It was exhilarating to witness! Education was easily accessible, with no limits.
In 2020, apart from the auditorium, our hospitals had no conference rooms built to host 50 residents while keeping them safely 6 feet apart. So, like everyone else, we needed to arrange our didactics in livestreaming sessions. This seemed limiting, at first. However, these live online sessions expanded our departmental didactics like never before. First, it gave us the opportunity to record all of the sessions, start a YouTube channel, and have all of our recorded lectures available for our on-call residents who missed them and for anyone interested from around the world. Second, we were able to invite speakers from all over the country, including our previous graduates. Third, residents were able to join our live sessions from our main training hospital, off-campus clinics, and their own homes (which increased our residents’ attendance rates). It was exhilarating to witness! Education was easily accessible, with no limits.
Saving your educational funds!
Virtual learning extended to medical conferences. Three years ago, I attended the American College of CHEST physicians conference in New Orleans, Louisiana. It was an exceptional experience that helped shape the physician I am today. In addition to experiencing the city of New Orleans and its rich culture, I was able to present my poster in front of a large audience, attend in person lectures from world-known clinicians, and participate in courses with hands-on procedural skills. This experience cost me $1000 from my educational funds, and 3 days of educational leave.
In comparison, over the past 2 years, I attended the American Heart Association and the American College of Cardiology virtual conferences. I was able to attend and present my posters in these conferences while covering in-patient service, and had access to all of the on-demand lectures for a total cost of $200. It was affordable, easily accessible, and did not cost me time off work.
Two years into this crisis, I find myself attending many conferences around the country through my screen. There has been an impressive advancement in accessibility to education through virtual reality, and we have pandemic to thank for that.
Telehealth
 According to the WHO, health inequity is defined as systematic differences in the health status of different population groups. As internal medicine residents, we have a weekly outpatient primary care clinic where we provide care for patients and follow up with them throughout our 3 years of residency. A large number of my clinic patients had co-existing mental health disorders that significantly affected their daily routines and lives. A part of our outpatient internal medicine training is to diagnose, treat, and follow up with patients who suffer from mental health disorders. A close and frequent follow up is a crucial part of the treatment plan to ensure the patients’ improvement.
According to the WHO, health inequity is defined as systematic differences in the health status of different population groups. As internal medicine residents, we have a weekly outpatient primary care clinic where we provide care for patients and follow up with them throughout our 3 years of residency. A large number of my clinic patients had co-existing mental health disorders that significantly affected their daily routines and lives. A part of our outpatient internal medicine training is to diagnose, treat, and follow up with patients who suffer from mental health disorders. A close and frequent follow up is a crucial part of the treatment plan to ensure the patients’ improvement.
Like any other residency clinic in the country, the majority of our patients were from a low socioeconomic class with limited access to transportation. In addition to commuting, they worked long hours, which made a monthly afternoon appointment and visit difficult. Required regular in-person follow-up sessions with patients were an obstacle to their treatment plans.
In March 2020, Michigan had the third highest number of recorded COVID-19 cases nationwide. Schools, workplaces, restaurants and the whole state closed to in-person activities and shifted to remote learning, home offices, and no-contact delivery. Like the rest of the world, our residency clinic was affected. Patients were scared of contracting the virus from the staff and other patients. Meanwhile, the staff felt a responsibility to contain this virus and prevent it from spreading. This allowed the opportunity for Telehealth to become the new normal where people felt safer talking over the phone, or through a video call with their healthcare providers. Telehealth opened a new door to fight health inequity. Patients have less obstacles to overcome to be able to follow up with their healthcare providers.
Front-line heroes
As the pandemic feels like it’s coming to an end with the mask-less faces at grocery stores, and lower numbers of COVID infected patients at the hospital. The world seems to have diluted the memories of the last 2 years we collectively experienced. As a physician however, I believe the difficulties we experienced were teachable moments we ought to learn from.
As the world feared an unknown virus, videos emerged of people yelling at others to maintain their distance or to wear masks, and hoarding toilet paper, I witnessed an exceptional culture of camaraderie in the hospital. I witnessed my co-residents volunteering to do extra shifts on the medicine floor as well as the critical care unit. Our family medicine residents offered to cover the extra load of patients on the medicine floor, our emergency medicine residents volunteered to help cover the critical care unit, and our surgery residents offered to help with procedures in the critical care unit. Residents spend long hours working as a team throughout their training years, this allows a sense of closeness, but this crisis pulled us even closer together as the heroes working against the pandemic on the front lines.
Thank you all for standing up to an unprecedented challenge in our lifetimes, and for your help over the last year!
May 18th, 2022
Will Interviews Stay Virtual? Hopefully, Yes.
Madiha Khan, DO
About 10 minutes into my virtual fellowship interview, I hear a whimper from under the desk. Confusion turns quickly into panic as I feel the tiny paws of my puppy grab at me for attention, and I realize she has somehow escaped her playpen and sneaked into my interview room. I try to keep my cool as I sit there in my tiny closet-turned-office, a small space with great acoustics but faulty door hinges, apparently. I consider coming clean immediately, but so many thoughts run through my head: What if the interviewer hates dogs? What if this is so unprofessional that it is seen as a red flag? (Or worse, if it’s seen as incompetence. If she can’t keep track of a puppy, how can she keep track of the wire during a cath?) I decide to keep the puppy’s appearance to myself and trudge on. Luckily, apart from some stiff answers on my part, the interview went fine.
I tell this story to my co-residents as we share our experiences from the fellowship interview season. Another resident shares her experience about when her apartment complex began testing the building fire alarm every few minutes during her interview: Each time she tried to answer a question, a loud siren would blare in the background. “Maybe they thought you were getting bleeped out by Zoom for cursing,” I said. Now that we have several thousand hours of collective Zoom/Webex hours under our belt, we can laugh and reflect on the growing pains of this past virtual fellowship interview season. Furthermore, despite some minor hiccups here and there, we agree on the benefit of the cycle being virtual, and we hope it stays that way.
As a PGY-3 chief recruiting for the next intern class while simultaneously interviewing for cardiology fellowship, I tried to take the positives from interviewing experiences of my fellowship-bound classmates and incorporate them into our own residency recruitment, while lobbying for the removal of the aspects that fell flat. Here are some reflections from the season, and insights as to why I hope this opportunity to improve a clunky, outdated process isn’t wasted by reverting back to in-person interviewing.
The Price of Admission
Applying and interviewing for the next step in your career shouldn’t be a financial undertaking. Removing the barrier associated with cost is an obvious advantage, not only for the financial well-being of applicants, but more importantly, for diversity and equity. Programs that were previously out of reach for applicants that may not have the financial ability to take flights, rent a car, and book a hotel on top of the base fees for applying to each program are finally within reach. Not to mention, there are only a certain amount of days allotted for interviews and carefully planning flights to not use more of your PTO than necessary is a stressor that won’t be missed. That is not to minimize the unique stressors of interviewing virtually (e.g., technical difficulties, securing an appropriate space to conduct the meeting) but I would rather battle Zoom fatigue than airline customer service for a delayed flight.
Is A 2D View Enough? The Culture Behind the Screen
Applicants have a few concerns with the virtual platform. Chiefly, they feel uneasy basing an opinion about a program and a city on a virtual interview day. After all, if you’re spending the next 3 years (or more) of your life in a city that is completely foreign to you, you probably want to see it. Most of the downside and hesitation stems from what may have been missed from the virtual display of interview day. Was everyone being honest, or was someone from the program standing behind the camera, staring the fellows down as they answered questions? Less obvious is the difficulty of picking up a stuffy vibe in the room. However, in my experience, asking the fellows candid questions generally yielded candid answers, especially if the program uses techniques like break out rooms where the setting was more intimate. Additionally, the virtual season actually allowed for more interaction with fellows, as people logged in from their cars, homes, or short breaks in the clinic to weigh in on their program. I actually think I got a better view on the culture of the program because of this feature. While the physical atmosphere is difficult to recreate in the 2D space, I found pre-made hospital tours (or impromptu walking tours) to be really helpful in that regard.
The Effect of Increasing Accessibility on Match Rates
Another issue is that of “interview hoarding.” For competitive specialties in particular, the concern is that top-tier applicants will over-apply and subsequently stockpile all extended interviews, thereby eliminating the trickle down effect of having interview spots open up where such applicants previously would have canceled. The simple answer to this would be to cap the number of interviews any one candidiate can amass, but the reality is much more nuanced, especially with the increasing competitiveness with each cycle. Also, the number of interviews needed to match differs for U.S. MDs, DOs, and IMGs. From a recruiting perspective, with such a high number of applications to sift through, adding more filters is the logical way to trim down the numbers to a digestible amount, which could adversely affect applicants that don’t fit stringent profiles. Moreover, after an interview, it’s difficult to gauge genuine interest if the applicant doesn’t have overt ties to the area or has never even been to the program’s city. Even if an applicant has serious interest in a program, having no ties appears to be a disadvantage that is underscored by a virtual cycle.
Troubleshooting Issues
Several specialties for the residency application cycle tried to account for these issues by implementing a supplemental application. Applicants indicated 2 out of 10 possible geographic regions in the U.S. as their preferences and then were able to send preference signaling tokens to a few programs of their choosing. Although it did circumvent some of the “pan applying,” it also offered up more areas of overthinking in a group of people who are particularly prone to overthink. At a glance, it would seem that signaling would increase the likelihood of getting an interview from that particular program, but it is hard to say how much of a negative effect not signaling has. Another proposal is to create a hybrid experience with virtual interviews having an in-person option. Though it provides the much desired facetime, it is hard to see a reality where the in-person applicants aren’t viewed more favorably, and even harder to imagine applicants willing to take that risk. A two-step process has also been suggested, where after the virtual interviews, a second round of limited in-person interviews is conducted in hopes of trimming down to those who are truly interested. Theoretically, this is more reasonable, but realistically, it prolongs the interview process where residents are already scraping together days off service to interview, and would now potentially have to use twice as much time.
Where Do We Go From Here?
Whether applications stay virtual, requiring programs to begin investing in social media to recruit the ideal fit, or if a reasonable combination is implemented (such as an in-person open-house prior to the start of the season or after ROLs are submitted), the moment of reckoning for the match system is here. Let’s not waste a pandemic! Let’s seize this occasion to reimagine a system for the future, even if it means experimenting for a few more cycles.
May 10th, 2022
“Look at Me …”: The Problem with Clinical Documentation
Khalid A. Shalaby, MBBCh
It was a couple of months into my second year of internal medicine residency. One of my patients canceled a 4 pm appointment. The spot was immediately filled with an urgent visit by another patient in our clinic. I had been working on improving my efficiency in the clinical setting since the start of my residency, and I had fallen into a rhythm of familiarity with our clinic, its staff, and our patients. Swapping a regular visit with an urgent care visit at the last minute was manageable.
I greeted my patient, asked if I could take notes as we talked, and started the visit. I listened during the “golden minute” — when the patient talks, uninterrupted, about what brought him or her to the clinic. The golden minute is a great time to connect with patients, listen attentively, and glean the most useful parts of the history that ultimately leads to an accurate diagnosis and treatment plan. During this time, I was typing on the computer in the examination room, when the patient said these three words: “Look at me.” His words hit me like a ton of bricks.
 The patient wasn’t angry or upset. He said these words graciously. He was merely trying to bring my attention to his hurting joint while I was typing parts of the HPI in an attempt to save time on documentation. I was so disappointed in myself. No patient ever had to ask for my attention while I was in the room since I started interacting with patients in medical school. I set the computer aside, actively listened, and carefully examined my patient.
The patient wasn’t angry or upset. He said these words graciously. He was merely trying to bring my attention to his hurting joint while I was typing parts of the HPI in an attempt to save time on documentation. I was so disappointed in myself. No patient ever had to ask for my attention while I was in the room since I started interacting with patients in medical school. I set the computer aside, actively listened, and carefully examined my patient.
Thankfully, he was my last patient of the day. Even though he was satisfied with the visit and glad to be seen on short notice, his words lingered and weighed heavily in my head. I sat down to reflect. How did I get to that point? How did I unlearn one of the core principles of being a physician, especially when I thought it was one of my strongest suits?
I could have come up with excuses, but they wouldn’t have been true. I was at fault. It dawned on me then that I had been gradually slipping away from patients and toward computers over the previous few months. My job satisfaction had also been declining. I was spending more time with computers and less time with my patients. Helping patients, spending time with them, and building rapport are the reasons I went into medicine.
 How extensive is the problem?
How extensive is the problem?
This issue permeates inpatient and outpatient care. Clinical documentation places a huge burden on all physicians, not just residents. U.S. physicians reported spending close to 2 hours daily completing documentation outside of office hours. This accounted for approximately 125 million hours in 2019 (NEJM JW Gen Med May 15 2022 and JAMA Intern Med 2022; 182:564). Many physicians multitask during their outpatient visits to mitigate the amount of work outside of their office hours. The data on use of computers during clinical encounters is mixed (Patient Educ Couns 2017; 100:50). In one study, more keystrokes during clinical encounters predicted less active patient participation (J Gen Intern Med 2018; 33:423). However, skilled and experienced physicians might still be able to maintain patient-centered communication during clinical encounters while using computers (J Gen Intern Med 2007; 22:43).
Although the burden of clinical documentation is grave, the onus is on healthcare organizations and physicians to honor what we were all taught — patients come first. Even though clinical documentation is indispensable, technology and innovation in electronic health records (EHR) should work for patients and physicians, not the other way around. There have been many local and national initiatives to have fewer clicks on computers, to get rid of unnecessary alerts or messages, and to lessen the burden on clinicians. We should continue those efforts and build upon them.
What practical approaches can we use to prioritize patients?
I do not aim to discourage anyone from documenting during clinical encounters. I just call on myself and my colleagues to be mindful of how it can affect our patients. Not every encounter will be the same. It may be feasible to document in some encounters. There are other appointments when we simply need to pull up a chair, have uninterrupted eye contact, listen carefully, and hold our patients’ hands. Many residents are eager to learn about clinical medicine but minimize the importance of improving their fluency with the EHR. Being proficient and efficient with the EHR is not a luxury but a necessity to deliver good patient care. On a personal level, I recognize that the less time I spend behind a monitor, the more I am able to be present at the bedside.
 There is always room for improvement. So I keep working on my patient-centered communication skills by learning from my co-residents, chiefs, and experienced attendings. I improve my ability to use speech recognition dictation technology, not just for dictation but for navigating the EHR. I customize the tabs on my EHR and add one-click shortcuts for most commonly used orders, which save me a lot of time, particularly on pre-rounding. On the inpatient side, I advocate for bedside rounding using computers-on-wheels. We are able to spend more time with our patients that way while using the computer not just to place orders but to review labs and imaging with patients.
There is always room for improvement. So I keep working on my patient-centered communication skills by learning from my co-residents, chiefs, and experienced attendings. I improve my ability to use speech recognition dictation technology, not just for dictation but for navigating the EHR. I customize the tabs on my EHR and add one-click shortcuts for most commonly used orders, which save me a lot of time, particularly on pre-rounding. On the inpatient side, I advocate for bedside rounding using computers-on-wheels. We are able to spend more time with our patients that way while using the computer not just to place orders but to review labs and imaging with patients.
There is no one formula for success. The most important factor is the dedication to patient-centered care. I for one have vowed never to hear those dreaded words again! I’ll always be looking at my patients.
May 4th, 2022
Insights from the AAFP Physician Health and Well-Being Conference
Mikita Arora, MD
Physician well-being has long been an issue in all medical fields, but especially in primary care — the concept of well-being is to heal the healers. Right now, this is especially important to those who have are burdened with burnout and the COVID-19 pandemic. A few weeks ago, I had the opportunity to attend the AAFP Physician Health and Well-Being Conference. It was a great experience. At the conference, physicians engaged at various workshops throughout the day to expand their ideas and to learn about wellness. Interactions at these workshops with wonderful physicians at different levels of their careers made me reflect on my own health and well-being. Here’s what I learned:
- Exercise, Exercise, Exercise
This is much easier said than done, especially during residency. The conference started each day with optional morning group walk, run, or yoga session. As a family medicine resident, I emphasize the importance of exercise all day long. However, how many residents exercise daily? I know if I have to choose between sleep or exercise, I pick sleep over exercise any day! Although it can be a challenge to make time for exercise during your busy schedule, it is important to make time for your own self-care and well-being. You don’t need a gym membership or fancy equipment. It can be something as simple going for a walk or going up and down the stairs at the hospital multiple times during your downtime.
- Everyday Mindfulness
Our words are powerful. Shifting our thoughts to something positive can make a huge difference. Something that I learned during the conference is to use “yes, and …” instead of “but, I ….” Although we often disagree with others, a simple change in two words can change a dreaded conversation into positive, meaningful one.
Another great tool to practice mindfulness is “catching” people doing well. Acknowledge and compliment them. This can truly uplift someone. The perfect example was mentioned in a previous NEJM Journal Watch blog post.
Gratitude journaling has been shown to decrease depression and increase happiness. Everyday, write down 3 things that you are grateful for that day — but you cannot repeat them! Read it a year from now, and you’ll be surprised by how wonderful your life truly is.
- Vent! You’re Not Alone!
During one of the workshops, we were asked to share with a small group a moment in our careers that still haunts us. One person on my table shared something that happened with one of his patients during his residency about 30 year earlier. His story gave everyone in the group chills and put tears in their eyes. He had not shared his story prior to that moment.
 Well-Being Isn’t Just for Family Medicine Physicians
Well-Being Isn’t Just for Family Medicine Physicians
Residency is a very challenging time in your career. Just remember that you’re not alone. One amazing resource that I discovered during the conference is PeerRxMed. It’s a free peer-supported program, designed to help physicians thrive both personally and professionally. You can connect with fellow physicians via weekly, monthly, and quarterly check-ins through text messages.
The AAFP Physician Health and Well-being Conference is not limited to just Family Medicine, either. Everyone is welcome to attend. I hope you can attend this conference (or one like it) at least once and experience all the great things it has to offer! Until then, prioritize your health and well-being. Just for yourself!
April 26th, 2022
Enjoy the Journey – You Deserve It
Brandon Temte, DO

Dr. Temte is a Chief Resident in Internal Medicine at Providence Portland Medical Center in Portland, OR
A few years back, I was a third-year medical student, exhausted on my general surgery rotation. I woke up at 4 am to the sound and smell of my coffee maker, muttering to myself, “only 1 week left.” I did not intend to become a surgeon, but I showed up early each day to get the best marks I could. Ready and driven, I threw myself into the demands of my work. After all, these were the days I had dreamt of as a first- and second-year medical student. I could remember sitting in class, enthusiastically waiting to be out in the clinical world. This experience is not unique. I am sure we can all remember times in medical school and residency when we looked to the future, just waiting for the current rotation to be over.
The Journey of a Medicine Trainee
 Most of our early career is about moving from one milestone to the next, reaching the next stage, and graduating. Whether it is completing medical school or the latest cardiology rotation, our early careers move us in increments of achievement. By nature, we are goal-driven professionals and reaching these accomplishments is what we do best.
Most of our early career is about moving from one milestone to the next, reaching the next stage, and graduating. Whether it is completing medical school or the latest cardiology rotation, our early careers move us in increments of achievement. By nature, we are goal-driven professionals and reaching these accomplishments is what we do best.
In medical school, we change jobs the way others change clothes. To start the month as a surgeon and end it delivering babies gives us the chance to sample the immense range of the human experience. But, that day in the operating room as a third-year medical student, busy counting down the hours, minutes, and seconds — I missed a genuine opportunity to enjoy the rewarding difference we made in a patient’s life.
My Journey
Exhaustion and inertia overshadowed many profound, beautiful, and educational experiences during my years of medical training. I focused on maintaining momentum, with an inability to pause. In retrospect, I was burned out and continuously grasping for the next ledge, no matter how small.
During times of rest and clarity, I would be able to find my stride and passion again. In times of prolonged fatigue, I would only look toward the future, unable to focus on the beauty of my journey. I would convince myself that it was all a passing feeling. It wasn’t until my second year of residency that a trusted faculty member said to me, “Brandon, you look burned out.” In a state of shock, I wanted to be defensive, but I finally let my guard down. This was one of the most important days of my medical training. Acknowledging my burnout changed my life and career. Since then, I have been more intentional about my day-to-day and more focused on how burnout can alter the journey.
Burnout — A Growing Concern
 The path we have chosen is long, and we are never done learning or achieving. Our entire careers are part of the journey, each stage is different but nonetheless an integral part. Physician and trainee burnout is a massive issue requiring intense continued discussion. At times, confronting burnout can feel like a hopeless task. Systems and organizations often drive the increasing mental health burden on our trainees and providers. The perceived lack of control and increased bureaucratic tasks can deprive us of our individual inspiration. In the most-recent (2022) report on physician burnout from Medscape, burnout was reported by 47% of physicians, up from 42% the year prior (Medscape 2022 Physician Burnout Report). This article is a personal recollection of my story so far, and we all have our own to share.
The path we have chosen is long, and we are never done learning or achieving. Our entire careers are part of the journey, each stage is different but nonetheless an integral part. Physician and trainee burnout is a massive issue requiring intense continued discussion. At times, confronting burnout can feel like a hopeless task. Systems and organizations often drive the increasing mental health burden on our trainees and providers. The perceived lack of control and increased bureaucratic tasks can deprive us of our individual inspiration. In the most-recent (2022) report on physician burnout from Medscape, burnout was reported by 47% of physicians, up from 42% the year prior (Medscape 2022 Physician Burnout Report). This article is a personal recollection of my story so far, and we all have our own to share.
Confronting Physician Burnout
 While we continue the critical discussions about physician burnout, take a few minutes to reflect on the amazing knowledge you gain and share each day. Consider the patients who have felt comforted and found solace in your care. Allow yourself to practice the gratitude you have earned, even for something as simple as showing up that day. When gratitude feels far away, and you’re having difficulty seeing through the fog, reach out to those around you. Take time to recognize your personal signs of burnout. They may be more subtle than you think. Our continued involvement in the discussion of burnout will help to protect the future of physicians.
While we continue the critical discussions about physician burnout, take a few minutes to reflect on the amazing knowledge you gain and share each day. Consider the patients who have felt comforted and found solace in your care. Allow yourself to practice the gratitude you have earned, even for something as simple as showing up that day. When gratitude feels far away, and you’re having difficulty seeing through the fog, reach out to those around you. Take time to recognize your personal signs of burnout. They may be more subtle than you think. Our continued involvement in the discussion of burnout will help to protect the future of physicians.
To all those simply surviving the latest rotation: you deserve to enjoy your journey.
April 19th, 2022
Calling out Impostor Syndrome
Abdullah Al-abcha, MD
As chief resident, I have been in a position to observe and mentor students, interns, and residents. I have always believed in the importance of recognition and support in a workplace. On a recent encounter with an intern, as I was praising her for her work, she responded rather unexpectedly! She thanked me for recognizing her, as
she still had doubts about how well she carries out her work. Her reaction was unexpected, because she excels in performing her duties. I would have never recognized that she felt this way — but then I reflected on my first year in residency.
My Experience
I was an international medical graduate (IMG) in a completely different world — functioning with my second language, practicing in a system I wasn’t familiar with, and little things, like the cultural differences in approaching patients. “Was my U.S. clinical experience good enough?” “Do I really deserve to be here?” Those were the thoughts that recurred throughout my first few rotations as I tried to become the person I was expected to be. Looking back now, I can’t imagine anyone saw those doubts in me. I probably looked like I was performing my duties competently while these feelings of self-doubt hid in the back of my head, showing up uninvited in moments of uncertainty or second thought.
It’s common for trainees to be nervous, it’s also common to question your competence when you’re reaching high-level achievements and are in a position to make important decisions, let alone life-altering decisions for others. It’s a very big responsibility, and it can weigh heavily on anyone working in healthcare. I told my intern that many of us have experienced these feelings during our journey — and I sent her an article about Impostor Syndrome.
 Impostor Syndrome
Impostor Syndrome
Also known as Impostor Phenomenon (because Syndrome can feel overwhelming, and it implies that it requires some kind of diagnosis or cure). A quick Google search of the words “impostor syndrome” brought up 7,380,000 search results, so to refine my search, I typed “impostor syndrome in healthcare,” which resulted in just 508,000 search results. Like everything else in our world, there is a vast amount of information about this topic, from medical research to self-help books, assessments, and tools to navigate this phenomenon. However, many people still don’t recognize that their self-doubt and feelings of inadequacy are part of this common phenomenon and that it’s prevalent among their peers as well.
Who’s at Risk?
Impostor Phenomenon was first described by Pauline Rose Clance and Suzanne Imes in 1978 when they reported their experience with highly successful women who reported a lack of internal sense of success. Research shows it’s prevalent, occurring in as many as 82% of professionals (J Gen Intern Med 2020; 35:1252). It’s crucial to note that these feelings can stem from being a minority in a workplace. The overwhelming feeling of being the first, the only, or one in a few in a workplace can raise self-doubt about reaching a certain position. Research shows that women, people from underrepresented minorities (URMs), and IMGs are more likely to experience this phenomenon (J Gen Intern Med 2008; 23:1090). Various tools are used to diagnose Impostor Phenomenon and to identify different types of impostorism. Some people suffer from these doubts throughout their entire careers, whereas others have episodes of increased feelings of impostorism as a response to different variables, such as starting a new job or getting a promotion.
Diversity and Impostorism
 I find it especially important to discuss impostorism now, as we move toward more diverse and inclusive workplaces. As the condition of Impostor Syndrome is defined, many people feel like their achievements or positions are due to luck rather than their hard work and qualifications. They fear being discovered to be less than they are perceived, and this can lead to anxiety, burnout, and depression. Rather than waiting for this cycle to unfold, it is important to implement protocols to ensure this is prevented. Especially considering the difference in prevalence due to demographics (i.e., women, IMGs, URMs), it is essential to raise awareness that some trainees could be affected more than others. Fortunately, change is happening: Leaders in different specialties are creating the necessary space for support and growth, such as diversity, equity, and inclusion (DEI) initiatives by the ACGME, as well as similar initiatives in institutions across the U.S.
I find it especially important to discuss impostorism now, as we move toward more diverse and inclusive workplaces. As the condition of Impostor Syndrome is defined, many people feel like their achievements or positions are due to luck rather than their hard work and qualifications. They fear being discovered to be less than they are perceived, and this can lead to anxiety, burnout, and depression. Rather than waiting for this cycle to unfold, it is important to implement protocols to ensure this is prevented. Especially considering the difference in prevalence due to demographics (i.e., women, IMGs, URMs), it is essential to raise awareness that some trainees could be affected more than others. Fortunately, change is happening: Leaders in different specialties are creating the necessary space for support and growth, such as diversity, equity, and inclusion (DEI) initiatives by the ACGME, as well as similar initiatives in institutions across the U.S.
I will begin my fellowship training in July, and as much as I look forward to this new experience, I anticipate feelings of self-doubt. However, I am now more prepared to navigate these feelings, because I have experienced them in residency and found ways to work around them.
 What worked for me:
What worked for me:
- Recognizing these feelings. I believe that this is the most important step, because once I knew what I was experiencing, those feelings became easier to manage.
- Sharing my doubts with trusted friends, colleagues, and mentors.
- Avoiding perfectionism and setting up a reasonable definition of success.
Wishing you good luck and positive self-talk on your residency and fellowship journey!
April 13th, 2022
A Glimpse of Being an IMG
Khalid A. Shalaby, MBBCh

Otterbein University Theatre & Dance from USA, CC BY-SA 2.0 <https://creativecommons.org/licenses/by-sa/2.0>, via Wikimedia Commons
“God on high, Hear my prayer
In my need, You have always been there
He is young, He’s afraid
Let him rest, Heaven blessed
Bring him home”
Jean Valjean praying for Marius in Les Misérables
I was back in my childhood bedroom on the outskirts of Cairo when I first met our wonderful executive editor and my fellow chief bloggers virtually. I was excited to start sharing some of my thoughts with the readers while, at the same time, trying to overcome the imposter syndrome feelings swelling in my chest. But mostly I was overjoyed to see my family again. This was my first time back in Cairo after 2 years and 3 months. I couldn’t help but think how representative this moment was of what it’s like to be an International Medical Graduate (IMG) in recent years. I do not claim to represent the voices of all IMGs, but I hope sharing my experience can shed light on some issues and possible solutions.
“Why did you come to the U.S.?” is a common question I am asked. The majority of the time, it’s out of genuine curiosity rather than implicit microaggression. At those moments, I ponder — what drives anyone’s choices in life? Probably running away from something or toward something else. It’s trying to avoid meeting our worst fears or chasing the stars.
A common misconception among the medical community in the U.S. is that IMGs are a monolith. But IMGs come to the U.S. for graduate medical education for many reasons — looking for a more humane, high-quality, structured graduate medical education experience that leads to a more predictable career path. We’re hopeful for a more fulfilling life and career — whatever that may mean to each of us. Some came to the U.S. as a legitimate pathway to immigration. Others are escaping wars, seeking reunification with their loved ones, or fleeing discrimination. We’re eager to learn about how the U.S. pushes the limits of science and medicine.
One quarter of licensed physicians in the U.S. are IMGs
Whatever that reason may be, the fact is, IMGs represent 25% of licensed doctors in the U.S., according to the AMA. More than half of IMGs who match in residencies every year, including 2022, are foreign nationals. This number is steadily increasing. IMGs are invaluable to the American healthcare system. That was perhaps most clearly elucidated when our visa status was in jeopardy due to a proposed rule change in 2020. This rule would have impacted “12,000 J-1 physicians engaged in training at approximately 750 teaching hospitals” and would have had a “devastating impact on U.S. patient care” according to a letter signed by numerous organizations opposing the rule that was eventually put on hold.
As foreign nationals, when we match into residency, most of us start an arduous process of paperwork to apply for a U.S. exchange visitor (J1) visa. This visa category encompasses many visitors to the U.S., is only valid for 1 year, and is not exclusive to physicians. Visas are renewed yearly in the physician’s country of origin’s U.S. embassy. A trainee can stay in the U.S. with the renewal of the ‘Certificate of Eligibility for Exchange Visitor’ (J-1) status (also known as DS-2019) but must renew the visa to reenter the U.S. should he or she exit.
In other words, many trainees need to travel to their home country every year, book an appointment with the embassy, and have an interview with a consular officer to renew their visa (although visa renewal by mail is an option in some countries). Before the pandemic, it was challenging to schedule vacation time in residency, align it with a visa appointment, and return to the U.S. in time. These challenges became almost insurmountable during the pandemic due to very limited appointments in U.S. embassies, travel restrictions, and other reasons. Leaving the U.S. during training, even for an emergency, without an appointment at one’s home country’s U.S. embassy, can jeopardize one’s training. Not to mention the risk of having an application in administrative processing that can take days to weeks. This has effectively deterred many foreign physicians in training from traveling to their home countries to avoid endangering their careers.
Some programs even gently advise their trainees against international travel during residency. This is mainly to avoid being ‘off-cycle’ in training, burdening their colleagues with their absence, and risking fellowship or job prospects. I can write pages on the angst of renewing a visa and my anxiety as I stood in line awaiting admittance to the U.S. embassy in Cairo. That simply should not be the case. U.S. GME training is so desirable that even if these conditions were to stay the same or get worse, it would still be in demand. So the main incentive to change and improve the process is U.S. healthcare institutions’ desire to make it less stressful for young physicians who undeniably deserve better.
Can the visa process be improved?
I cannot begin to fathom the complexities of the U.S. Immigration and Customs Enforcement or the requirements to safely grant someone a U.S. visa. I can only speak to how difficult my experience has been over the past few years. Like many aspects of our lives, the pandemic has uncovered the inadequacies of administrative systems. Visa issuance for IMGs is certainly one of them. Can this process be streamlined? Physicians in training may need a separate visa category that’s tailored to their needs. Other countries, like the U.K., have implemented visas for healthcare workers. Could visas be renewed in the U.S., where we live all year long? Could the yearly renewed DS-2019 suffice as proof for maintaining lawful status if we got a visa for the duration of residency?
I realize that there are many pressing issues in the U.S. and around the world. I understand that, as a society, we have a finite capacity for empathy. It is not lost on me how privileged I am to remain employed at an excellent institution. However, having lived in the U.S. for the past few years, I have learned that we should not settle for mediocre but strive for excellence, that reform only happens when we speak up until our voices are heard, and that tenacity, solidarity, and empathy are core features of the American character, not temporary fads. ECGMG, AMA, and other organizations have advocated for foreign physicians in training. We need to amplify these efforts.
What can GME programs around the country do, while we advocate for a better process?
- Having an excellent Training Program Liaison makes all the difference in the world!
- Faculty members, please check on IMGs in your program, especially those who have not seen or visited their families for months or years. We are all acutely aware of the stressors of residency, and separation from loved ones adds to these.
- Be as flexible as you can with vacation requests to renew visas (within reason), and understand that it’s a difficult process.
- Don’t shy away from choosing excellent IMG candidates. I can assure program directors that, despite the hassle, we’re well worth it! We’re grateful and appreciate the opportunity.
For medical students and residents, I would recommend the following:
- When interviewing for residency or fellowship, choose a program that will actively support you.
- Surround yourself with your local “family” in the U.S. My UConn family has kept me going throughout the pandemic. I couldn’t be more thankful.
- Residency is incredibly busy. Schedule the time to stay connected with your loved ones. There’s nothing more important.
- Plan ahead! Plan your vacations and your visa appointments. Stay on top of your paperwork. It does not always work out the way you intended, but if you don’t plan at all, it will be more difficult.
It’s overzealous of me to compare bringing IMGs to their home countries to renew their visas to Jean Valjean dragging the wounded French revolutionary, Marius, to safety in Les Misérables. But that’s how these words touched me as I listened to them again, after a long period of absence from home. If you don’t agree with my take, I hope you can at least enjoy Colm Wilkinson’s angelic voice as he sings “bring him home.”
I realize that this essay and my experience are Middle East/North Africa centered. I recognize that IMGs from other regions of the world face unique challenges. Please share your experience and any suggestions you may have.
April 5th, 2022
#MedTwitter: The Good, the Bad, and the Surprisingly Useful
Madiha Khan, DO
“Does this look professional enough for Twitter?”
My co-resident holds up her phone to show me her newly minted Twitter profile. A picture of a distant, shadowy figure in sand, framed by a circular thumbnail, is her profile picture. Underneath this vague portrait is what could only be presumed to be her twitter handle: her initials followed by a series of 6 or 7 numbers.
“This… looks like a bot’s profile.”
Despite having a decade-long dalliance with Twitter, I was reluctant to join the MedTwitter space, which (to a Redditor like me) sounded akin to a stunted faux-LinkedIn profile. However, about 2 years ago when I started my foray into digital education, my mentors in this realm over at CardioNerds seemed to view it as a necessary medium in the quest for creating decentralized, open-access medical education. So, I dusted off my decade-old account, deleted my tweets to AT&T regarding their customer service, and set sail. Fast forward to today, and I truly believe it is an invaluable resource. After revamping our residency twitter page, successfully convincing unwilling residents to join, and even ghost-writing a few bios, I wanted to share some insights on the benefits and pitfalls of being a part of the platform.
Why Should You Join?
By and large, the greatest return on investment is for those seeking residency or fellowship positions. I get it — in a time where trainees are expected to be productive researchers, effective educators, and excellent clinicians, it seems unjust to ask us to be our own brand ambassadors, too. But the truth is, more and more national organizations and programmatic leadership are seeking out the social diplomats of our time to usher us into this inevitable digital era.
The rise of social media ambassadors for conferences, for spotlighting and disseminating research, and for frequent posting of open positions are a testament to the fact that being able to navigate this space is viewed as a necessary skill. With the world available at the push of your fingertip, networking possibilities are infinite, even without flagrant self-promotion. Speculating further, from a program’s point of view, it doesn’t hurt to be a familiar face in a stack of endless applications. However, in my experience, this is probably not as much of an advantage as is being perceived as a conscientious ‘professional’ social media user.
Perhaps the most valuable aspect (and the primary reason I remain on the platform) is the medical education content. The latest research, journal clubs, “Tweetorials” on various topics, and the resultant discussion from experts in the field is the true value of this community. I was surprised to see not only the vast number of leaders in medicine, but also how active they were in sharing their knowledge and experience (which may underscore the need to have a presence on social media even for those well established in their field). What once was privileged access to information and people is now open; there is no more gatekeeping. The leaders of medicine, and of our world, are just 280 or fewer characters away.
There are some very effective teachers too; I find myself referring to certain Tweetorials by faculty across the country just because they explained how to approach a diagnostic dilemma so well in 5 to 10 tweets. The opportunity to have a virtual seat in other program’s teaching rounds — without having to watch an hour-long YouTube video — is pretty surreal.
And of course, another reason to join is to follow everyone’s favorite ophthalmologist, Dr. Glaucomflecken:
Why You May Have Avoided MedTwitter…
The medical community on Twitter is a bubble. That’s what makes it so easy to use as a networking tool, especially within your specialty, but it is also what makes it a vulnerable space. Certain ideas and personas are over-amplified in the echo-chamber of Medtwitter, and the space is particularly prone to groupthink. In a place where people are eager to break through, honest opinions that are not considered part of the mainstream are suppressed and, at worst, posters are sometimes “canceled” entirely. Unfortunately, this leads to behaviors like humble-bragging, self-aggrandizing, and virtue signaling, which are as easy to identify as they are off putting. Not to mention, just because someone is famous on MedTwitter doesn’t always mean they are as approachable and supportive to their colleagues in real life. The differing realities can make the community feel disingenuous.
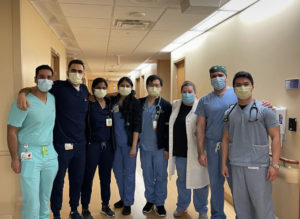
Furthermore, sometimes a post may get some unwanted attention from someone outside of the community. An innocent picture of a group of residents getting the vaccine may diverge from the usual algorithm and show up in the wrong feed, and you end up with jarring comments from strangers calling you an agent of big pharma. It can be unnerving, especially for those who haven’t dealt with trolls before.
Personally, I try to avoid anything outside of the educational content of the bubble. I do this by being deliberate with which tweets I interact with and/or retweet to keep a semblance of control over ‘the algorithm.’ When it comes to the inevitable unwanted comments, I will impart age-old advice that was passed down generations of my family: Don’t Feed the Trolls.
Final Thoughts
Let’s face it, being a trainee on social media is complex. For the most part, medical students/residents/fellows potentially have the most to gain from being in the space with networking opportunities, digital education, and ability to keep apprised of advancements in their field in an efficient and interactive way. The key is to take it at your own pace. It doesn’t really matter if you want to interact peripherally with a de-identified account as a picture of sand or build an online presence, so long as you get value from it, and Don’t Feed the Trolls.
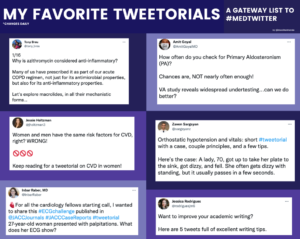
If you’re on the fence, here are some threads I keep coming back to (links included below):
- Why is azithromycin considered anti-inflammatory? By @Tony_Breu
- A practical approach to primary aldosteronism by @AmitGoyalMD
- CVD in Women by @JHoltzman3
- Tips for orthostatic hypotension by @sargsyanz
- Differentials for VT by @InbarRaber
- Academic writing tips by @rodriguesjm6
BONUS posts:
- Iron studies simplified by @sargsyanz
- Prophylaxis tips by @sargsyanz (and the NEJM article here)
- Really anything by @gradydoctor
May 17th, 2021
“Feel the Musicality”: How Do Surgeons Learn?
Vivek Sant, MD

Dr. Sant is a General Surgery Chief Resident at NYU Langone Health, Bellevue Hospital, and Manhattan VA in New York, NY.
My friends and I spent Thanksgiving 2018 attending surf school in Jacó, Costa Rica. We spent that week fully immersed in twice-daily surf sessions interspersed with conditioning, balance exercises, and of course, downtime to explore the town and rainforests of Jacó. Having been on a surfboard only a handful of times previously, this was a new experience for me. Our surf instructors quickly got us out on the water, and onto wave after wave, helped us start to stand up on our surfboards. During video review of one of our surf sessions, our head instructor explained to us that the key to surfing was to “feel the musicality.” While I noticed a few raised eyebrows in response, this exhortation immediately resonated with me, through my experiences learning other skills, as well as through my surgical training.
My mentors often remind me that the learning that happens in residency is only the beginning of a lifelong journey: 20 years into practice, 80% of the procedures one will be performing will be ones learned after residency. Of course, 5 years of surgical training provide a firm foundation, but how does one develop the tools to learn more easily, efficiently, and constantly? In residency, we need to learn how to keep learning. As I have cultivated other hobbies and skills over the years, I have found common themes emerge regarding how I learn best. These themes overlap significantly with how I have approached my own surgical training.
In college, I took up guitar. I was largely self-taught, from online tutorials and YouTube videos. I can still remember going from being barely able to curl my fingers around the guitar fretboard without significant pain, to playing my first chord, to eventually strumming through an entire song. I practiced the riffs from Sultans of Swing so many times one summer, that my family still cannot hear that song without a visceral reaction. I would occasionally hit a wall while practicing. I would practice 40 or 50 repetitions on a particular riff and still not have it come out perfectly. The next day I would wake up, pick up my guitar, and find my fingers able to effortlessly play the same riff I had been struggling with the previous night. Time after time, I have found this process repeating itself. Get the repetitions in. And then keep the faith. In surgical residency, especially in the early years, I found myself practicing a certain maneuver or procedure, wondering if it would ever make sense — and with practice, over time, it always has.
In the summer of 2017, I set my sights on a lofty goal — sailing a boat in the Mediterranean to Santorini. The only obstacle? I had no idea how to sail. But how hard could it be to learn? I started by taking two weekend-long courses — the American Sailing Association 101 and 103 courses, Basic Keelboat Sailing and Basic Coastal Cruising. I then went on numerous practice sails with an instructor to gain experience, and took an extensive online sailing theory course, learning about docking in various winds and currents, basic engine repair, and the effects of the sun and moon on tides and the weather. As my eyes opened to the vast body of knowledge I would have to master, Santorini seemed to be falling farther away from me, so I set an intermediate goal — sailing a boat by myself, locally. That fall, a friend and I solo-chartered a sailboat in Key West for a week. As prepared as I was from my courses and practical training, nothing could have truly prepared me for that final leap of independence. With no one to fall back on for advice, a new phase of learning commenced, and I grew tremendously from this experience. In surgical training, opportunities for independence result in tremendous surgical maturation, and in my chief year, I have come to greatly appreciate these opportunities.
One of the hobbies I pursued in medical school was ice skating, toward my larger goal of learning how to play ice hockey. A medical school classmate took me to buy hockey skates and then took me out on the ice for the first time. Like learning to ride a bike, there was a significant disconnect between watching others glide effortlessly on the ice and doing so myself. I would wake up early on Sunday mornings, watch ice skating tutorials online, then take the subway down to Bryant Park and practice for a few hours. I learned quickly that words and instructions are only a coarse approximation of a complex set of moves that you ultimately have to feel out, discover, and eventually master for yourself. In early sessions, with the benefit of a beginner’s mindset, I could fall on the ice multiple times and think nothing of it. But as I progressed, I found myself trying to avoid falling, and in the process, risking less and advancing less. So I resolved that I would lay it all on the line and push myself until I fell at least once every session. In surgical training, similarly, I have found great value in embracing discomfort. Leaning into the discomfort that accompanies a lack of knowledge, technical skills, or expertise and pushing past it has motivated me to grow tremendously. In residency, every 4 weeks, when we finally become comfortable on a service, we are whisked away to the next rotation, so we continue to progress, advance, and learn.
What exactly is this musicality one feels when surfing, sailing, ice skating, playing guitar, or even performing surgery? With a surfboard under your feet, you strive to feel a oneness between your mind, body, feet, surfboard, waves, and the ocean at large, so that you feel the exact right moment to get up on the board and drop in on a wave. Instead of having to think through the complexity of which way to turn the sails, tiller, and boat, given the wind angle, point of sail, and direction you want to go, you instead feel the water streaming past the tiller of your boat and the pull of the wind on the sails and instinctively push the tiller in just the right amount and direction needed to adjust your course. Instead of focusing on how the tutorial video said to “make c loops on the ice with the inside edge of your skates,” you relax and instead feel the traction between your feet, skates, and the ice, and the balance of your body, and adjust your position as needed to continue the motion you want. Your brain no longer has to calculate what key a song is in, figure out what notes are part of that scale, and then what frets and strings are used for that scale; instead, your fingers move to make music and express the song coursing through your mind! But how do we get to this joyous unconscious stage of expertise? How do we use our surgical instruments as unconscious extensions of our fingers and hands, and learn to separate tissues in accord with their natural tissue planes, in the beautiful dance that is surgery? Embrace the discomfort. Put the repetitions in. Then, keep the faith. And with humility and grace, in that final leap to independent practice, you’ll find yourself more than capable of serving your patients.