May 25th, 2022
The Pandemic Through a Rearview Mirror
Abdullah Al-abcha, MD
Throughout medical school, the word pandemic was something distant from our world of advancements. We truly believed we had reached the epitome of a future where a virus is something we could contain. COVID-19 proved us wrong. In March 2020, the World Health Organization (WHO) declared a pandemic. An unprecedented event that would change our world. An epic event that we considered to be something of the past forced us to hurry into a virtual future we all feared. Many people were overworked, others lost their jobs, and too many lost people dear to them.
As healthcare workers, we were affected like everyone else, but it was our role to fight the pandemic — face to face — on a daily basis. As with all unfortunate events, it’s odd to speak about the good side of the COVID-19 pandemic, but it has altered our profession in unconventional ways: Everything from seeing patients virtually in their own homes to attending conferences around the country from the comfort of our couches.
Learning at your convenience
During the first year of the pandemic, I was serving as the junior chief resident. My responsibilities involved arranging our departmental weekly didactics sessions, but everything was different, everything was virtual! Rereading this sentence, it seems normal and insignificant, as we were already headed toward a virtual world (despite everyone’s fears) for many years, so it shouldn’t have been a surprise — but in reality, it was. In addition to life occurring mainly through screens, when we did see people, we had to maintain a distance of 6 feet apart. It felt impossible, given the congestion of the world we were used to living in.
 In 2020, apart from the auditorium, our hospitals had no conference rooms built to host 50 residents while keeping them safely 6 feet apart. So, like everyone else, we needed to arrange our didactics in livestreaming sessions. This seemed limiting, at first. However, these live online sessions expanded our departmental didactics like never before. First, it gave us the opportunity to record all of the sessions, start a YouTube channel, and have all of our recorded lectures available for our on-call residents who missed them and for anyone interested from around the world. Second, we were able to invite speakers from all over the country, including our previous graduates. Third, residents were able to join our live sessions from our main training hospital, off-campus clinics, and their own homes (which increased our residents’ attendance rates). It was exhilarating to witness! Education was easily accessible, with no limits.
In 2020, apart from the auditorium, our hospitals had no conference rooms built to host 50 residents while keeping them safely 6 feet apart. So, like everyone else, we needed to arrange our didactics in livestreaming sessions. This seemed limiting, at first. However, these live online sessions expanded our departmental didactics like never before. First, it gave us the opportunity to record all of the sessions, start a YouTube channel, and have all of our recorded lectures available for our on-call residents who missed them and for anyone interested from around the world. Second, we were able to invite speakers from all over the country, including our previous graduates. Third, residents were able to join our live sessions from our main training hospital, off-campus clinics, and their own homes (which increased our residents’ attendance rates). It was exhilarating to witness! Education was easily accessible, with no limits.
Saving your educational funds!
Virtual learning extended to medical conferences. Three years ago, I attended the American College of CHEST physicians conference in New Orleans, Louisiana. It was an exceptional experience that helped shape the physician I am today. In addition to experiencing the city of New Orleans and its rich culture, I was able to present my poster in front of a large audience, attend in person lectures from world-known clinicians, and participate in courses with hands-on procedural skills. This experience cost me $1000 from my educational funds, and 3 days of educational leave.
In comparison, over the past 2 years, I attended the American Heart Association and the American College of Cardiology virtual conferences. I was able to attend and present my posters in these conferences while covering in-patient service, and had access to all of the on-demand lectures for a total cost of $200. It was affordable, easily accessible, and did not cost me time off work.
Two years into this crisis, I find myself attending many conferences around the country through my screen. There has been an impressive advancement in accessibility to education through virtual reality, and we have pandemic to thank for that.
Telehealth
 According to the WHO, health inequity is defined as systematic differences in the health status of different population groups. As internal medicine residents, we have a weekly outpatient primary care clinic where we provide care for patients and follow up with them throughout our 3 years of residency. A large number of my clinic patients had co-existing mental health disorders that significantly affected their daily routines and lives. A part of our outpatient internal medicine training is to diagnose, treat, and follow up with patients who suffer from mental health disorders. A close and frequent follow up is a crucial part of the treatment plan to ensure the patients’ improvement.
According to the WHO, health inequity is defined as systematic differences in the health status of different population groups. As internal medicine residents, we have a weekly outpatient primary care clinic where we provide care for patients and follow up with them throughout our 3 years of residency. A large number of my clinic patients had co-existing mental health disorders that significantly affected their daily routines and lives. A part of our outpatient internal medicine training is to diagnose, treat, and follow up with patients who suffer from mental health disorders. A close and frequent follow up is a crucial part of the treatment plan to ensure the patients’ improvement.
Like any other residency clinic in the country, the majority of our patients were from a low socioeconomic class with limited access to transportation. In addition to commuting, they worked long hours, which made a monthly afternoon appointment and visit difficult. Required regular in-person follow-up sessions with patients were an obstacle to their treatment plans.
In March 2020, Michigan had the third highest number of recorded COVID-19 cases nationwide. Schools, workplaces, restaurants and the whole state closed to in-person activities and shifted to remote learning, home offices, and no-contact delivery. Like the rest of the world, our residency clinic was affected. Patients were scared of contracting the virus from the staff and other patients. Meanwhile, the staff felt a responsibility to contain this virus and prevent it from spreading. This allowed the opportunity for Telehealth to become the new normal where people felt safer talking over the phone, or through a video call with their healthcare providers. Telehealth opened a new door to fight health inequity. Patients have less obstacles to overcome to be able to follow up with their healthcare providers.
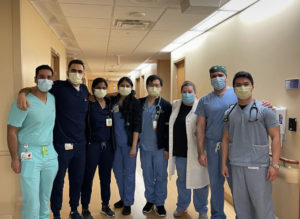
Front-line heroes
As the pandemic feels like it’s coming to an end with the mask-less faces at grocery stores, and lower numbers of COVID infected patients at the hospital. The world seems to have diluted the memories of the last 2 years we collectively experienced. As a physician however, I believe the difficulties we experienced were teachable moments we ought to learn from.
As the world feared an unknown virus, videos emerged of people yelling at others to maintain their distance or to wear masks, and hoarding toilet paper, I witnessed an exceptional culture of camaraderie in the hospital. I witnessed my co-residents volunteering to do extra shifts on the medicine floor as well as the critical care unit. Our family medicine residents offered to cover the extra load of patients on the medicine floor, our emergency medicine residents volunteered to help cover the critical care unit, and our surgery residents offered to help with procedures in the critical care unit. Residents spend long hours working as a team throughout their training years, this allows a sense of closeness, but this crisis pulled us even closer together as the heroes working against the pandemic on the front lines.
Thank you all for standing up to an unprecedented challenge in our lifetimes, and for your help over the last year!



Thank you for sharing your experiences! I was a Family Practice physician for 35 years but had retired 2 yrs before the pandemic so this indepth look into medical residency & practice in this pandemic age was truly appreciated. Sending it on to others I feel would be interested. Thanks again.