March 5th, 2020
Should We Avoid Exposing Residents to Coronavirus?
Eric Bressman, MD

Dr. Bressman is a Chief Resident in Internal Medicine at Icahn School of Medicine at Mount Sinai in New York, NY
The arrival of the novel coronavirus to the U.S., and the inevitability of its eventual spread, raises an interesting question: Should we avoid exposing residents to the virus?
 Before we try to answer this question, we should start with some important qualifiers. While a good deal about this novel virus remains unknown, the majority of cases appear to be low risk, particularly for the demographic of the average resident. Furthermore, if this outbreak does reach pandemic levels, exposure to healthcare workers of all levels ultimately will be unavoidable. Finally, even with the best of protocols in place, it will be impossible to triage out every potentially infected patient at the point of first contact.
Before we try to answer this question, we should start with some important qualifiers. While a good deal about this novel virus remains unknown, the majority of cases appear to be low risk, particularly for the demographic of the average resident. Furthermore, if this outbreak does reach pandemic levels, exposure to healthcare workers of all levels ultimately will be unavoidable. Finally, even with the best of protocols in place, it will be impossible to triage out every potentially infected patient at the point of first contact.
With all this in mind, COVID-19 may not be the best case study, but it’s an interesting opportunity, nonetheless, to pose a broader question regarding the role of trainees during epidemics and pandemics.
History
Let’s start with a brief historical overview of this question. Physicians have always been at the frontlines of deadly outbreaks, and as a result, were regularly infected by the same diseases as their patients.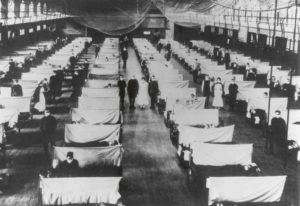 The first century of U.S. history can be recounted in a sequence of epidemics, from yellow fever to cholera to typhoid fever. In an era of unregulated medical and graduate medical education, and limited understanding of the spread of these diseases, there was scarcely any thought given to the protection of students and trainees during these outbreaks.
The first century of U.S. history can be recounted in a sequence of epidemics, from yellow fever to cholera to typhoid fever. In an era of unregulated medical and graduate medical education, and limited understanding of the spread of these diseases, there was scarcely any thought given to the protection of students and trainees during these outbreaks.
Graduate medical education evolved over the course of the twentieth century from a mix of apprenticeships and a limited number of more structured programs, to a landscape of predominantly hospital-based internships, and eventually specialty-focused residencies with a unified accrediting body. Important questions that persist to this day were considered during this time, including the place of the resident on the spectrum from student to employee.
The AIDS epidemic was likely the first major infectious disease outbreak during which the unique experiences of students(Health Educ Res 1999; 14:1) and residents (Ann Intern Med 1991; 114:23) were explored, although the emphasis tended to be on the duty to treat in spite of the fears and perceived risk. In the intervening decades, however, the vulnerability of the trainee has been reconsidered, and this has shifted the conversation. By the time of the 2014 Ebola epidemic — although different in scale and mode of transmission from HIV — much wider efforts were undertaken to protect trainees from potential exposure, prompting a healthy debate (Acad Emerg Med 2015; 22:88).
Pros
We can entertain a couple arguments in favor of trying to protect residents from a potential pandemic exposure:
- The infection control argument: Because residents are mid-level providers, any patient a resident sees will also be seen by a supervising attending. To limit total number of exposures and mitigate the potential for disease spread, the fewest number of providers possible should see any at-risk patient.
- The student versus employee debate: During the Ebola epidemic — which was vastly different from the current pandemic — nearly all medical schools forbade students from providing care for rule-out Ebola cases (Acad Emerg Med 2015; 22:88). There may not be one unifying theory about why these policies were developed, but the reasons probably include insufficient training, liability, and a less than clear moral imperative. Conversely, faculty are compelled to care for all patients, at times even in the face of personal risk, by virtue of their training, their contracts, and their professional codes of conduct (Am J Bioeth 2008; 8:4). The question, as always, is where residents fall on this spectrum; this has been argued both ways over time, often according to what is most convenient for the employer.
Cons
At the same time, some real downsides might occur in trying to shield residents from potential exposures:
- Missed training opportunity: This is especially true when it comes to outbreaks that require rigorous infection control practices, as was the case with Ebola. If rule-out protocols exclude trainees, health systems will be less likely to invest resources in training them. This may, in fact, put residents at higher risk, both now and in the future.
- Modeling professionalism: Residency is about attaining not just the knowledge and skills, but also the attitudes, necessary for life as a physician. At times, this encompasses embracing some risk in the service of our patients. Whatever the status of residents — student, employee, or student-employee — there might be value in imparting this message.
Conclusion
The role of the resident during a pandemic raises interesting questions; although they generally operate at the front lines, the instinct is there to protect them when personal risk is involved. COVID-19 might not be the best case study for a number of reasons, but it is more than just a thought experiment. Health systems are developing protocols at this very moment, and the role of trainees will be an essential consideration. In some instances, the protective instinct of a particular attending might be to handle the rule-out cases personally. But most importantly, the next pandemic might pose even greater risk, and it will be all the more essential to find the right balance between expectation, education, and limitation.



After AIDS was identified, we made care safer for both patients and staff by increasing protection against blood-borne pathogens. Now is the time to use concern about COVID to increase protections against healthcare-associated respiratory infections. If care is unsafe for residents, it is unsafe for others and we need to make it safer. Sick residents and healthcare workers need to stay home. This will a require a culture change, replacement staff and paid sick leave. Pre-waiting room, we need to screen routinely for respiratory symptoms room patients in private rooms. We need to research our infection control measures of respiratory hygiene to develop evidence based ones. What PPE really matters? Could strict use of adequate ventilation, gloves, mask and hand hygiene prevent cases or are goggles and gown always needed? Every facility is at risk for nosocomial respiratory infections, non-ventilator pneumonia is often the most common nosocomial infection. Flu attacks every year. Let’s use COVID as the basis for broader, enduring respiratory protection for patients and staff.
Dear Dr Bressman
Thank you so much for your informative article, I am a PM&R (physical medicine and rehabilitation) resident in Tehran, Iran.
Since the novel CoVID 19 epidemic has been announced, the university hospitals replaced some of the admission wards with Corona patients ward, Respiratory Emergency ward, and respiratory triage section; also, every single intern or resident – no matter in which field!- is obligated to work shifts in each Corona ward, and as an inexperienced group of residents in respiratory cases, all of us (PMR, neurology, radiology,radiotherapy, nuclear medicine, pathology, orthopaedic surgery, neurosurgery,…) are now exposed; although we are not even quite competent to manage these cases.
I would be grateful to know your expert opinion on this matter.
Thank you so much
Nafisseh Jafarian
My view is that residents are qualified doctors and as part of clinical teams, they should be exposed to the infection prevention and control training as their attending physicians. Once they have been trained in infection prevention and control practices as the rest of the team, for the two reasons listed under Cons – i.e. training opportunities and modelling professionalism, my view is that they should be exposed to any patient that comes through as the rest of the team.
However when it comes to undergraduate medical students in clinical rotations, my view is that they should not be exposed in the front line as they are not yet qualified doctors.
Residents are in a highly compromised position, with low pay, more patient exposure, and less rights. Attending physicians must be on the front lines with residents if this is going to work. Otherwise, I fear residents will quickly recognize the flagrant inequities at play and may chose to step aside.
Importantly, resident training is limited to a few year period, and needs to remain focused on resident education when alternatives exist. This means that if coronavirus wards are developed, they should be run by attending physicians, rather than pulling residents away from critically vital elements of their education.
As a resident, I disagree with those that say we should be shielded from dealing with this pandemic. A key part of our education is learning to cope with situations such as these. Avoiding our involvement would jeopardize our ability to handle similar pandemics in the future. Full opinion here:
https://medium.com/@joshdhorton10/to-be-a-partner-in-life-physician-surgeon-training-during-the-covid-19-pandemic-45f66780d4ae?source=friends_link&sk=b8467361d239dc349b052d0924ac7e1b
What are your thoughts on dental residents being pulled to the COVID task force? There has been a big divide in some of our departments regarding this. George Banks mentioned key points in the above comment. Dental residents, while still paid a PGY salary, are also paying tuition (60% of salary before taxes) back to the hospital at the same time. They are working with Covid patients in medical centers with no prior experience of ever even being in a hospital setting, not learning anything related to their own field of study (but paying tuition), and pressured to do things they’re uncomfortable with… all the while their attendings stay at home giving these orders.
PGY-2 IM Resident here.
I am in favor of minimizing exposure to all healthcare workers, including residents. If attendings are going to see the patient, there is no need for residents to go into the room.
As for the above arguments, this Pro that I mentioned above is the only objective point that has been mentioned. Both of the cons that are mentioned are theoretical and weakly founded points as I will explain:
Missed training opportunity: I beg to differ. What are we missing? Learning how to wear a gown and gloves? We do the same when we see influenza patients. Learning how to hand wash? No, there is no missed training opportunity, this is utterly ridiculous. Anyone can learn the PPE procedures. Even the techs have to follow them, so there is nothing unique here that residents need to risks themselves being exposed to learn. Also, when a pandemic happens, most residents in programs across the country are not adequately trained, but are just handed masks and told to gown up and go, while the hospital administration is in a panic trying to figure out what to do and how to handle the situation and supplies are running low everywhere. This is a pretty bogus argument point.
Modeling professionalism: Ok, this again like I said, is very theoretical and is non-objective. Professionalism is why we need to go into the room and be exposed? Tell to the residents who become COVID positive, to those who develop symptoms, and to those who end up getting tubed as has happened in some cases. This is another ridiculous argument. Professionalism is a subjective concept. Who says that attendings are in general more professional than residents? And professionalism is though by exposing residents to a potentially lethal disease where that exposure is unnecessary? Seems like a pretty foolish argument.
If residents are unnecessarily exposed, it’s not the resident potentially getting sick that is the worst part, it’s the thought of being asymptomatic, which most younger individuals may be, and then going around and unknowingly passing COVID on to other healthcare workers, nurses and elderly patients. This is a very OBJECTIVE assessment and is probably the only real point that needs to be considered in this discussion. the attendings are going to see that patients regardless so there is no need for residents to go into the room. The above cons seem to be something out of a classic administrative play book by someone who is just interested in running their hospital and making profits. Unfortunately that is what is happening on the ground.
Residents are being forced to work the Covid units and be exposed to high viral loads over and over again, especially if they are not staying on at that particular hospital after they graduate. How many residents have to die before this is changed. They have no choice unless they want their career ruined forever…