May 12th, 2016
Birth Control Without Rx: Will Women Get the Care They Need?
Scott Cuyjet, RN, MSN, FNP-C

Scott Cuyjet, RN, MSN, FNP-C, practices adolescent medicine in the San Francisco Bay area.
A new law went into effect in California on April 1 that enables women to receive a birth control prescription from a pharmacist. A similar law has been in effect in Oregon since the beginning of the year, but there is a significant difference between the two states’ laws. According to an article by The Pew Charitable Trusts, “The California law is more expansive than Oregon’s. It allows pharmacists to prescribe a vaginal ring and hormonal birth control shots in addition to pills and patches that release hormones through the skin.” The authors also state that access would be improved given that “93 percent of Americans live within five miles of a pharmacy.” While I applaud the increased access that will most likely decrease the unintended pregnancy rate, which hovers around 50%, I also have some concerns.
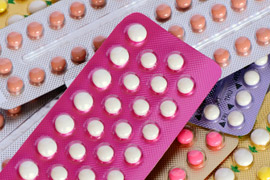 My biggest concern with the California law is that new and follow-up patient visits regarding birth control methods are a great opportunity for health care providers to screen for relationship abuse, converse about issues around sex and pleasure, and screen for sexually transmitted infections. If patients are seeing a pharmacist instead, these elements of care either won’t be done because pharmacists do not have the capability, or they won’t be done well.
My biggest concern with the California law is that new and follow-up patient visits regarding birth control methods are a great opportunity for health care providers to screen for relationship abuse, converse about issues around sex and pleasure, and screen for sexually transmitted infections. If patients are seeing a pharmacist instead, these elements of care either won’t be done because pharmacists do not have the capability, or they won’t be done well.
I am also concerned that one visit to the pharmacist is not enough to reinforce teaching of how to use patients’ chosen birth control method and what to do if they mess up. For pills, patches, and rings, I see my patients back in 6 weeks for follow-up, and at that time I check on side effects and review with them when to refill and what to do if pills are missed or a patch or ring is not placed on time. I also discuss how to get refills and why prescriptions are only good for a year, as that is time to follow-up.
For Depo-Provera shots, will the pharmacists only start administration if patients are in their first 5 days of menses, or will they do quick starts and see them in 2 weeks for a pregnancy test? For their follow-up Depo-Provera, will they only give patients their shots between weeks 11–13 after the first shot, or will they be able to utilize the off-label schedule of up to 17 weeks later?
Another concern is that some women, despite the Affordable Care Act, still don’t have insurance for primary care and should also receive primary-care screenings. Given how busy pharmacists are, judging from how long it takes my patients to get a prescription filled after I send it (1–2 hours, depending on the pharmacy), I am not sure how pharmacists are going to make time for the cursory screenings they are supposed to do.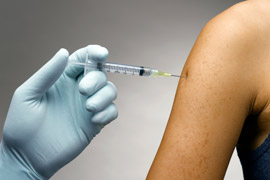
Based on my web research, the pill is available without a prescription in most parts of the world. This is where I think advocates and pharmaceutical companies have their sights set. In California, this was the path to Plan B (the morning-after pill) becoming an over-the-counter (OTC) medication. The problem with OTC medications is that you cannot pay for them with your insurance, and some of them are expensive, which still limits access. When Plan B was still on patent, it was about $50 over the counter. Now, if a woman plans ahead and buys emergency contraception from Amazon, she can find it for as low as $25.
I think we could best decrease the unintended pregnancy rate through improved access if the pill, the patch, the ring, and emergency contraceptives were OTC and insurance covered their cost.
Categories: In the News, Patient Care, Policy
Tags: birth control, California, contraception, healthcare access, pharmacists, prescriptive authority, unintended pregnancy
You can follow any responses to this entry through the RSS 2.0 feed. Both comments and pings are currently closed.
32 Responses to “Birth Control Without Rx: Will Women Get the Care They Need?”

NP/PA Bloggers
Elizabeth Donahue, RN, MSN, NP‑C
Alexandra Godfrey, BSc PT, MS PA‑C
Emily F. Moore, RN, MSN, CPNP‑PC, CCRN
Advanced practice clinicians treating patients in a variety of settings and specialties
Learn more about In Practice: Reflections from NPs and PAs.
-
 NEJM Journal Watch — Recent General Medicine Articles
NEJM Journal Watch — Recent General Medicine Articles NEJM Journal Watch — Recent Pediatrics and Adolescent Medicine Articles
NEJM Journal Watch — Recent Pediatrics and Adolescent Medicine Articles-
Tag Cloud
- addiction adolescent health advanced practice provider clinical role Communication compensation deep brain stimulation diagnostic test discrimination Emergency Medicine empathy end of life Falls Geriatrics gun violence Haiti healthcare access health care quality humanity intensive care intracranial aneurysm legislation lifestyle modification longterm care Massachusetts medical knowledge negotiation neurosurgery NPAEP obesity opioid abuse Parkinson's disease patient-provider communication patient navigation pediatrics performance personal growth practice privileges primary care professional title retirement running team-based health care toxic work culture Vaccination

So your argument begins with “we need to follow-up and assess these patients, pharmacists can’t adequately perform this task” but then your closing argument is “the pill should be OTC.” I don’t really follow your logic.
Hi James,
Obviously I am conflicted about this, which is why I have presented both sides. On one hand I think patients initiating a birth control method should be assessed and followed at least initially, but there is also the issue of the unplanned pregnancy rate around 50%, which is somewhat due to restricted access. Through writing this post I have processed this and come to the conclusion that what is best for the patient is improved access even though it means they will not have any follow up unless they ask for it. That is given they can afford it or someday insurance covers it OTC.
Thank you for reading and helping me clarify this.
Scott
My 4 year doctorate degree in pharmacy and 8+ semesters of pharmacology and pharmacotherapy have more than prepared me to counsel patients comprehensively regarding birth control or any other medication for that matter. I find it narrow minded that you think a phamacist will not be capable of screening, counseling, and having adequate conversations with our patients. Pharmacists will be able to follow up as soon as that 28 or 84 day supply is out allowing us a great opportunity to interact with the patient. Even when a pharmacy is busy I have never met a pharmacist that will not take the time to counsel their patients. Patient care needs to come before turf battles.
PharmD,
Thank you for reading and taking the time to reply. This is not a turf battle. I am free to discuss my concerns about changes in law and policy as it relates to my practice just as you are free to comment. Please read my reply to Emily and Stacy.
With that said I must give a frequent example of pharmacists educating patients or the lack thereof. I often have patients come back who I have directed to do a quick start on their OCPs in the middle of the week. When they return they were either told to start the first Sunday after their next menses or were not told about the stickers in the pack to relabel their medications and were starting in the middle of the week and having to remember to go back to the beginning of the pack before taking their placebo pills.
Ultimately I am about patient access and in this case reducing unplanned pregnancies. If this or OTC access is the answer, then great! I am sure there is much more pharmacists want to do professionally and can do.
Thanks!
Scott
Scott,
As a pharmacist I agree that in a retail setting it is not possible for pharmacists to perform well-woman exams, though I feel that this is an area where pharmacists can work as a valued member of the health care team to ensure adequate follow-up is obtained. My main concern regarding your article is your following statement: “I am also concerned that one visit to the pharmacist is not enough to reinforce teaching of how to use patients’ chosen birth control method and what to do if they mess up. For pills, patches, and rings, I see my patients back in 6 weeks for follow-up, and at that time I check on side effects and review with them when to refill and what to do if pills are missed or a patch or ring is not placed on time. I also discuss how to get refills and why prescriptions are only good for a year, as that is time to follow-up.” To me this sounds exactly like what a pharmacist does. It is the primary role of our profession to educate patients on proper use and potential side effects of medications. When a patient is being counseled by a pharmacist and reports an intolerable side effect it is the role of the pharmacist to work with the patient and prescriber to find an alternative therapy. As the medication experts in the health care team I feel that you grossly underestimated our contributions in your article. While I agree that follow-up does need to be done with a PCP, I would hope that you would place more value on pharmacists as a member of the health care team and utilize the wealth of medication knowledge that they possess.
Sarah,
Thanks for reading and responding. Please see my response to Emily, Stacy and PharmD. I have nothing against pharmacists and appreciate what they do, although as I mentioned in my other response that I may not be fully aware of all that they do or are capable of doing. I will work on this. I put it out there that pharmacists do the same in regards to us providers so we can form better relationships and maybe improve care to our patients in the process.
Scott
Hi Scott,
While I can understand where your concerns arise based on the average person’s perception of what a pharmacist does, I would like to take the opportunity to remind you that we are the medication experts. It is more than just counting by 5 and ringing a cash register. Your concerns over counseling patients on medication use and side effects are unsubstantiated, as that is one of our primary duties for ALL medications. Through our extensive education on all things pharmaceutical, we have acquired an intimate knowledge of pharmacology and therapeutic applications. Combine that with communication skills that we have refined through school, practical experiences, and (for many pharmacists) years of working as technicians in the pharmacy, we are more than up to the task. Another of your concerns is follow-up. You say that you see your patients 6 weeks after starting therapy? Most hormonal contraceptives come in 28-day supplies, which means they are back at the pharmacy in 4 weeks. This presents the perfect opportunity to have a conversation with the patient, which is as easy as “flagging” the patient for required counseling upon pickup. Computer systems at most community pharmacies do for patients getting a new medication or changing a dose. On top of that, patients would have to come back at least every 3 months to pick up refills, which means we see the patient far more often than a prescriber who writes a 1 year prescription and the patient doesn’t follow up until it expires. This gives us more opportunities to follow up beyond initiation. The reason prescriptions take 1-2 hours to fill is mostly due to system backup…escripts are not instant, and when they do come through, they often get triaged behind more acute prescriptions. Above all other duties, patient counseling always takes priority. Plus, expansion of pharmacy services like this often prompts participating pharmacies to expand staff to accommodate the demand. The final concern of yours that I would like to address is the use of methods outside of “the pill” and transdermal systems. When programs like this are implemented, they come with appropriate education and certification programs. Pharmacists aren’t going to just go at it blindly, interpreting instructions like an IKEA dresser. Expanded pharmacy services require extensive training through continuing education provided by national pharmacy organizations, in which we learn about the medications and practice the administration techniques for certification. The most standardized example of this is immunization training. Once upon a time, the thought of getting a flu shot at your local pharmacy was unheard of…now it is the standard, with the multi-step APhA training course built into most student curriculums. I assure you that pharmacists who take this opportunity will be appropriately trained. The fact is, pharmacists are a woefully underutilized health resource, and have been for many years, resulting in a diluted version of the pharmacist’s role in health care. Not every pharmacist will be comfortable with these duties, especially those who have lost a good portion of their clinical knowledge from being limited for so many years. New graduates are in a prime position to take this on, though, with fresh clinical experiences and education. We have the knowledge and we have the skills, we just need the opportunity to make a broader impact on our communities.
Stacy,
Thank you for reading and such a through response. Please see my reply to Emily as it covers much of what you have addressed.
I appreciate having pharmacists and would like them to be more autonomous as they are an underutilized resource. In the articles I have referenced and read it states that the pharmacists are going through training to do this expanded service. I did not think they were just “going at it blindly”. It sounds like you are up for the challenge as I am sure many pharmacist are, but as you stated I also think there are many who like to stay behind the scenes.
Thank you.
Scott
I would like to point out that many of the things you mentioned pharmacists were not capable of (counseling on appropriate use of birth control, safe sex practices, side effects of medications, need to refill/medication adherence) are exactly the things I see as a pharmacist that are not being done by our physicians and other providers. This is contraceptives and all other medications. Most patients show up at my pharmacy with a prescription not knowing what it is, what it is used for, how to take it, when or how to refill, or what side effects they may experience.
I think you are receiving such a strong response from pharmacists because we are not the problem but the solution.
Pharmacists are more qualified than any other profession to counsel a patient on use of medication, adherence, and how the medication will affect them and we are rigorously trained in how and when to refer patients when they need medical care including exams or changes in therapy.
Please, talk to some pharmacists! Understand how pharmacists and other providers can work together to provide expanded and more quality care to all patients.
Thank you for reading Amanda and Touche! There are good and not so good people in all professions. I am sorry if my wording was offensive. I did not mean it to be. I will try to be more careful in future posts. It was nice to have a dialog between NPs and pharmacists though.
Scott
I understand your concerns but I disagree with many of your conclusions.
Most patients see their pharmacist much more often than any other healthcare provider, allowing for many more opportunities for follow up, to check on side effects and adverse effects, and to make recommendation regarding when to see a primary care provider.
As a pharmacist in a busy urban pharmacy, I have had many conversations with women of all ages regarding their sexual health, healthy relationships, and signs and symptoms of sexually transmitted diseases. Some of these patients have even stated that their primary care provider never asked them about any of the previous issues.
Further, so many of my uninsured or Medicaid patients are only able to go to free clinics or extremely busy community health clinics with healthcare professionals who are only their for a short rotation and never have an opportunity to develop relationships with their patients — while I do since I see them much more often, and for years and years.
Another point of concern you mention is regarding drug counseling and the pharmacist’s ability to give the patient all the necessary information and speak with them about their concerns. You say that you “check on side effects and review with them when to refill and what to do if pills are missed or a patch or ring is not placed on time. I also discuss how to get refills and why prescriptions are only good for a year, as that is time to follow-up.” My question here is, what do you think pharmacists do now? These questions and topics are what I go over with every patient, especially someone who has a new prescription or a new disease. This is what I teach my pharmacy students and residents to ask when counseling patients.
Again, I understand your concerns. But I am troubled by the apparent lack of knowledge regarding the practice of pharmacy.
This new law is a win for public health and women’s health. As a healthcare professional, I would hope that you will support the successful implementation of the new regulations and be a champion for your patients and pharmacists.
Emily,
I appreciate your reading and taking the time to reply. As a disclaimer my sister-in-law, who I like and respect professionally, is a pharmacist. You sound like a pharmacist that is very thorough and takes time to counsel their patients. I am curious as to where you are able to talk to patients about their sexual health and relationships. Whenever I have been to a pharmacy all the counseling is done at the window and is not private. When I go to the pharmacy I mostly deal with the techs, but look around and observe what is going on. I do not see pharmacists taking blood pressures or checking a patients weight because they have complained of weight gain on their medication, nor have I heard them giving diet and exercise counseling. Occasionally I will speak to a pharmacist on the phone who goes above and beyond to help a patient, but mostly I get them dumping back on me as the primary provider and it appears that the pharmacy staff is overwhelmed. I will go to my local CVS, Walgreen’s, and Rite Aid and will have a conversation with the pharmacists about the other things they do in order to not have such a skewed view about pharmacists since I spend most of my time in clinic bubble.
I agree this is a win for public health and women’s health and I am supportive, but I also I think it is acceptable to have a conversation about my concerns with a change in law and practice.
Thank you.
Scott
Thank you for this article. Like you, I am an NP who feels somewhat conflicted about OCs being prescribed by a pharmacist, but I also want women to have easy access to birth control to prevent pregnancy. And like you, I am concerned about follow-up, which gives me the opportunity to discuss side effects, what to do if a pill is skipped, etc. Sometimes the patient’s blood pressure is elevated after starting OCs, and that needs to be dealt with. And of course, it lets me reinforce the absolute necessity of not smoking.
I did not know, and was surprised to read, that California permits pharmacists to prescribe Depo-Provera, which of course, is a long-acting hormonal treatment with multiple indications and which can have many side and adverse effects. I would love to hear from a pharmacist about whether they have concerns about taking on the risks and liabilities of prescribing Depo-Provera or any other hormonal birth control method, for that matter.
Loretta,
Thank you for reading the blog and your thoughtful reply. I do like to recheck their blood pressure and there can be a lot of follow up in person or by phone to manage the irregular menses that can come with Depo shots.
Scott
Hi Loretta,
As a pharmacist, I have many of the same concerns about risks and liabilities regarding Depo Provera as you do as an NP. It would never be a first line choice for me for a patient due to concerns regarding side effects of a long acting medication and also potential for bone thinning, but it potentially could be the right choice for a select few patients (most of whom I would probably refer to primary care due to risks of lack of follow up). I don’t know of any pharmacists who would consider the Depo shot risk-free. Much as I know few NPs or DOs or MDs who would consider Depo risk-free.
Michelle, RPh
Thank you Michelle for responding to Loratta’s request about Depo Provera.
Scott
Hi, Scott –
Interesting comments (mostly from female pharmacists) and replies.
As a pharmacist, I, too, am a bit conflicted about pharmacists injecting Depo-Provera and being able to do adequate follow-up. But, it’s probably OK. Any pharmacist who wants to “prescribe” contraceptives must first take extensive continuing education to ensure they are knowledgeable about all aspects of such prescriptions and how to counsel and follow-up with patients. (And, of course, they’ve already taken many courses in pharmacology, etc. before they get their PharmD.)
As you note, you practice in a “clinic bubble” (a somewhat unique environment), and so likely have more time in your workday schedule to do counseling and follow-up than the average pharmacist does. However, CA laws and regulations now allow pharmacists/pharmacies to be reimbursed with “extra money” if they perform services like what we’re discussing. It’s important that employers staff pharmacies adequately so that they do have time to perform effective counseling, etc., and this is already happening in many places.
Pharmacists are the most accessible healthcare professionals, and, as in Oregon, CA pharmacists will make sure that patients are adequately counseled and receive appropriate follow-up, probably better than what patients would receive if they get a contraceptive Rx from their PCP in a more typical setting than where you work.
Tom,
I am not sure about the relevance of mentioning that the comments and replies are “mostly from female pharmacists” and think you could have made the same points without that statement. However, I appreciate the information about pharmacists bringing in more money for the pharmacy with these new visits. It makes me wonder if this is actually access driven, or if improved access was just the catch phrase that the owners of these companies used to justify lobbying for this change to increase revenue.
As I mentioned in some of my other comments I am going to talk to some local pharmacists to see how and where they are going to have these conversations that go beyond how to take a medication and it’s possible side effects. I appreciate that you folks are everywhere, but that does not mean you are set up for private conversations.
Thank you for reading the blog and for taking the time to respond.
Scott
Scott, I mentioned female pharmacists since (1) this is an issue re: women, and (2) Many female patients will feel more comfortable talking with a female pharmacist. But, certainly, a male pharmacist should be able to put a female patient at ease and conduct counseling, etc. just as effectively.
Again, you work in a “clinic bubble”, unlike most of the real world where women are prescribed contraception by PCPs (with very little decent clinical counseling). I’m a little leery of your plan to go out and talk unrandomly to pharmacists, without a well designed written plan approved by PharmDs and MDs (and other NPs). The way you stated your “plan”, it would likely be a clinically meaningless “pseudo-study”. Hopefully you can work with others to develop a meaningful study.
I probably should have also mentioned that you should consult with researchers and/or statisticians who know how to properly conduct a meaningful study.
I’ve published over 2 dozen peer-reviewed articles and chapters in medical, pharmacy and nursing journals and textbooks, as well as teaching at schools of pharmacy, medicine and nursing.
I wish you the best in your pursuits.
So, in your mind it’s okay for a physician to be reimbursed for knowledge based services, but not a pharmacist? You literally think our job is to only put the pills in a bottle? Why did I go to school for 8 years if I’m not supposed to use my brain?
Response to Jimmy, PharmD:
I’m not sure how you got that interpretation from my comment. As I’ve previously mentioned, pharmacists who undergo special training in CA should and can get special reimbursement for providing these clinical services. I agree with you. Perhaps you made a mistake re: who your response should be to.
Gosh, this feels short-sighted. Weren’t similar arguments made about nurse practitioners in the not too distant past. And talk about competing arguments: women need counseling about abuse but women can’t afford insurance. The single biggest boon to a woman’s future is to control when and if to be a mother. I really hate to say this/be devisive; however, a male writing about his concerns about highly qualified pharmacists giving women what they desperately need when private practice primary care (let’s not even discuss OBGYN pricing) fails them smacks of paternalism.
Erin,
One, thanks for reading and taking the time to comment.
Two, I never said anything about women not being able to afford health insurance.
Three, I am a feminist and am all about women’s choice and being able to control their bodies. The clinic I work at does not fail women and most of our patients come in for Family Planning. Just because I write about a change that is occurring does not mean I am trying to block it.
Lastly, yes the AMA and some of it’s members had and still have issues with how much a nurse practitioner should be able to practice under supervision and independently. However, the role of the nurse and then the nurse practitioner has always been direct patient care. My personal and professional experience with outpatient pharmacists is they don’t council every patient who comes in for a refill and check on side effects. Most people get an initial consultation depending on the medication, but usually only see a tech to get their medication or have it mailed to them. People also have the option to waive their consultations and I would bet many of them do.
Thanks!
Scott
Scott, I invite you to touch base with a local pharmacist who is clinic-based. I do not work in a clinic, but some pharmacists do, alongside doctors, physician assistants, and nurse practitioners. Sometimes these pharmacists go by the term “MTM pharmacists”. Please do ask around and see if you can find one locally to meet; they have education beyond a PharmD typically (one to two years of residency) and would most definitely check patient’s blood pressures, weights, etc, based on side effects they are monitoring for. This may open your eyes to an area of pharmacy you haven’t seen before.
As a pharmacist who is not clinic based but practices in a tradition pharmacy role, I can assuredly check a blood pressure myself, and have advised patients based on blood pressure numbers in the pharmacy to contact their PCPs for medication changes. While my current pharmacy is not set up to give patients birth control in a safe manner, many of my colleagues work in places where this would not be a problem. The key is ensuring that patients are receiving the care they deserve. Being a pharmacist shouldn’t limit this care; it’s mostly about the work environment and must be individualized to each location as to what can be offered to patients to ensure they achieve indicated, effective and safe outcomes.
Michelle,
Thank you for reading and your reply. Hopefully this blog has started a conversation. I will talk to more pharmacists and hopefully they will seek out providers to see all the things we do other than send a Rx to their pharmacy.
Scott
Most pharmacy students today get a pretty good view of inpatient non-pharmacist provider work. In my rotations, I rounded daily with medical teams and worked alongside the medical residents in their workroom. This is pretty standard today. Some students also get to spend time with outpatient non-pharmacist providers during rotations, but this is less common.
Thank you. We should spend more time getting to know each other as professionals and people.
I think the point is that, with training in school, plus the state-required extensive post-graduate training for pharmacists in the states they can now prescribe birth-control measures, they have more than adequate training in physical assessment, etc. to allow them to prescribe the most appropriate form of birth control for a given patient.. It takes pharmacists 8 years of geing a full-time student, plus post-graduate training after they get their doctorate to do what they do. They are also smart enough to know that, if they work in a less-than-conducive environment, they will refer a patient to a healthcare professional (pharmacist, etc.) who can provide the appropriate birth control services.
I have to agree with the other pharmacists who commented, you severely underestimate our knowledge base and scope of practice. Furthermore, I have never met a pharmacist who is not willing to call a physician in the interest of providing quality patient care. I just want to re-echo what you said, this is not a turf battle. If a patient came in who has been using the Nuvaring for over a year with no complications, was in a monogamous relationship, and just needed a refill, why should I have to refer that patient to you or any other provider to have her prescription refilled? It’s inconvenient and costly for the patient! If a young patient came in, who had never been on contraception before, it would be in my best professional judgement to refer that patient to an OB/GYN for consultation. I have no shame in making sure that my patients have access to safe and reliable care. You’re right, I don’t have time to do a well woman check up, but if I, as an independent healthcare professional, judge that necessary, I am more than willing to put my ego aside and refer out in the best interest of my patient’s health and safety.
Oh, and by the way, it doesn’t always take 2 hours to fill an Rx. It takes however long it needs to take without causing the patient bodily harm. Drugs are dangerous, and last time I checked, my job was making sure that they don’t kill patients. You have no business worrying about my pace or workflow. In the rare scenario when it takes more than two hours to fill an Rx, let me explain why:
-You see a patient in clinic.
-You tell your medical assistant what to call in or you hastily punch an error ridden scrip through your e-scribe software.
-Your MA goes to lunch or gets distracted and doesn’t send the scrip for an hour and a half, or we get a scrip full of errors.
-The patient shows up and asks why their prescription isn’t ready.
-We tell them we haven’t received it or their was an error in the scrip and we need to call your office in the best interest of their safety. The patient is now angry as all get out and wants all of my attention.
-i call your office and talk to your MA. She has no respect for me as a provider and thinks I’m on her level (i.e.: I don’t have a doctorate, I have a junior college certificate). She says she’ll talk to you.
-You finally get around to calling me back because you are just as busy as I am (you know, because your patients wait an hour in your clinic waiting room just like they wait an hour for their scrip at my pharmacy).
-You’re rude to me on the phone because you have no respect for me as a provider. You hastily acknowledge that there was an error or the scrip has not been sent and you give me a new Rx verbally. I read it back as quickly as possible because I respect the fact that you have patients to see.
-I fill the scrip in 15 minutes.
-The patient has now been waiting for two hours when in all actuality, it could have taken 15 minutes.
So next time you feel like demeaning my profession, think about what we do to make sure the right drugs get to the right patients.
First of all, I want to thank you for bringing this important topic to the minds of medical professionals. It was indeed a surprise to find out this law had already been passed and in the process of going into effect. I have surveyed several of my pharmacist colleagues after reading this blog and I have yet to find one that knew about this upcoming new change. As a pharmacist that works in a retail setting, clinic setting and acute care hospital, I have a strong passion for advocating the clinical expansion of the pharmacists’ role (in addition to the dispensing and basic consulting expectation). I have no doubt in my mind that certain trained pharmacists are clinically capable of taking on the responsibility of birth control dispensing and clinical screening. In addition, pharmacists do have direct access to patients which is one of the essential needed components to decrease unplanned pregnancies.
That being said, it is not without serious doubt that I think our profession is ready for this change. As I had mentioned, many retail pharmacy colleagues of mine had no idea that this law had passed and will soon go into effect. Which begs the question –have we as pharmacists been given the proper tools and training to prepare for this change in the community?
In addition, not all retail pharmacies have the correct operational set up to privately consult patients on this important matter. There has been a big push to obtain consulting rooms near the retail pharmacy for in-depth private conversations, however this has not yet been accomplished in many pharmacies. One of the pharmacies I work at has a very small consulting area at the end of the counter and I am positive that this would be a HIPAA violation given the fact that many people are at hearing distance. Privacy is particularly important when it comes to a topic as sensitive as sex.
Another barrier that pharmacists face when taking on this new clinical role is the current expectation to complete their daily tasks at hand. We would be ignorant if we ignored the fact that we as pharmacists receive much financial pressure to fill a certain par level of scripts in a certain specified period of time (error-free), while the phones are often ringing off the hook. Unless, there is a serious operational change from the retail pharmacies, then we are setting ourselves up for failure. What I mean by operation change for example, is to have a clinical pharmacist on duty who can provide these additional services. Until this change occurs, we are not in a position to meet all of these patient expectations.
Furthermore, I would be naïve to think that certain colleagues of mine would be interested in speaking to young women and girls on the topic of sex. This is a very sensitive subject and not all pharmacists possess the comfort level needed to not only dispense birth control, but to become aware of these patients’ sexual behavior and potentially screen for sex abuse. Can pharmacists be trained to conduct such consultations?—sure, however the issue at hand is not only access but also a need to offer a safe forum for these select patients to feel comfortable enough to seek out these available services. Not all pharmacists would be the clinician of choice for these topics. Sure, we can say that only pharmacists who are interested would obtain the extra certification, but if patients are given the expectation that any pharmacy would provide this service, I can foresee that all pharmacists would be required, if not strongly recommended to be able to dispense these class of drugs. If the certified pharmacist is not available, the pharmacy would be losing money on birth control prescriptions.
Scott, you are right that screening might be compromised in the retail setting. Given the right tools, the right resources and a pharmacist with the right personality, would pharmacists would be effective counselors on this issue? —Of course. Unfortunately, all of those components are not currently in place. You, however do this for a living. You have committed your professional career to counseling girls and women on sex, birth control and any issues surrounding this topic. As a pharmacist I am passionate about medication safety, and any medication-related conversations, but counseling patients on sex and sexual abuse would be something out of my personal convert zone. It would take additional training and education to provide the correct tools needed to have an effective consultation on this issue. I am, however always excited for pharmacists to have more opportunities for direct patient care and for the profession as a whole to gain the trust from patients and the community needed to take on this important additional role—my fear is that drastic changes need to be done in the retail setting before we can have a successful implementation of this law.
Finally, our goal is increased access for patients, a decrease in unplanned pregnancies, and a safe and open forum for this discussion with patients. Medical professionals as a whole should come together to accomplish this task. I am not suggesting that retail pharmacies are not the right place, I am just highlighting the fact that drastic measures need to be taken in order for pharmacists to be the only point of contact for birth control. I am looking forward to the changes that will be taking place and I thank you for bringing this topic to light. Much more discussion to come I presume…
Thank you Suzie for reading and your contribution to the discussion. You have made some good points that we all as providers of patient care should think about.