January 12th, 2021
Vaccine [Rollout] Reactions — In Support of Residents
Stephanie Braunthal, DO
During the first week of the U.S. national vaccine rollout, news outlets reported a protest after a major medical center’s initial COVID-19 vaccine distribution list did not include almost the entirety of their house staff. Less publicly, I have heard about additional instances across the country where trainees as a whole have been or felt excluded from receiving a dose from the first shipment of vaccines. A common trope among the stories in which the slight was accidental has been that, somewhere along the line, nonmedical staff misunderstood the role of medical trainees in patient care, did not know where they belonged administratively, or in one case, did not know the difference between residents and fellows and inadvertently left the former off the communication, even though a substantial number actually were due to be vaccinated.
Hearing about such clerical errors reminds me that the hierarchy of academic medicine is not intuitive to those outside of the field. For the most part, the result of this is fairly benign, and usually results in explaining things to friends and family (such as the difference between residency and fellowship, or that, as an internist, I haven’t delivered a baby since medical school). For patients, not understanding the hierarchy can create confusion and even frustration. They want to know why they need to wait to meet the attending physician in a teaching clinic, or why they can’t get a medication refill after discharge by the resident who took care of them in the hospital.
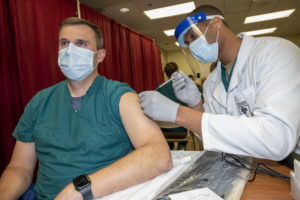
Doctor at Walter Reed National Military Medical Center receives a COVID-19 vaccination. Dec 14, 2020. (DoD photo by Lisa Ferdinando) CC BY 2.0
Residents and fellows can also be negatively affected by others misunderstanding their role. Their confidence can be shaken when a patient demands, “I want to see the doctor,” when they enter the room (not knowing that they had been mislabeled as a student); or they might feel alienated if they don’t have a workspace on a rotation because they are not formally employed by that department. Building up over time, these types of seemingly harmless encounters make many trainees feel like they do not belong or are not appreciated in the place to which they devote so much of their lives. Unfortunately, these perceptions were amplified for those who were not included in the COVID-19 vaccine rollout, no matter how unintentional the slight(s) may have been.
So, what will help trainees trust that their programs, institutions, and patients value and respect them? After reflecting on my own and my peers’ experiences in their programs, transparency, equity, agency, and recognition appear to be fundamental. Some suggestions of ways to implement these principles include:
- Deliver honest and consistent communication about operational matters directly to house staff.
- Offer the same opportunities to trainees as are given to hired employees (e.g., retirement matching, health benefits, vacation time, and appreciation weeks).
- Ensure residents and fellows understand where they fall in both the educational and administrative framework, such that they are aware of all the channels by which they can direct questions and advocate.
- Include residents and fellows in institutional initiatives that affect them.
- Devote time during orientation of nonphysician employees to the structure of medical education. Ensuring that other healthcare providers and administrative colleagues understand the different roles of physicians will not only improve teamwork, it will also help them communicate with patients on our behalf.
- Recognize trainee efforts and accomplishments publicly.
These measures not only contribute to wellbeing and morale, they also engender a higher likelihood of retaining the resident or fellow after training.
One of the lessons I have learned in my short time thus far in program leadership is that sometimes asking how we can support is as important to intuitively providing support. The vaccine rollout has sparked meaningful conversations about what it means to feel valued and respected in one’s place of work, particularly as a trainee. My hope is that the dialogue continues beyond the pandemic and results in lasting change.




Thanks for addressing this small matter as an example of a larger issue. However, from my experience as a medical student, intern, and resident, I’ve never seen evidence that such treatment was attributable to lack of intuitive awareness or clerical mistake, any more than 36 hour shifts were. The best way to create a sense of arrogant entitlement is to force the individual to undergo a prolonged formative period of powerlessness and organizational disparagement, It’s as essential to the reproduction of the traditional culture of medicine as it is to the traditional culture of the Marine Corps.
Stephanie, this post is spot on re: helping residents feel valued. I think involving residents in institutional / leadership committees, as you mention, is a way to accomplish a lot of these goals. It helps us housestaff feel valued and involved, have our voices heard, and keeps us apprised of developments in a timely fashion!
Thanks Stephanie for writing about this important issue! In the age of COVID-19, it has become even more apparent that a large proportion of the direct patient care is provided by trainees/ residents. Alongside other frontline staff, residents should be afforded the same workplace protections and also be in the first/ priority vaccination group.
The other misunderstandings of residents’ role, I think is a larger issue related to the culture of an institution and although these misunderstandings may be unintentional, I would categorize them as microaggressions against the trainee from patients or staff. I think in particular in the inpatient setting, bedside rounding can remedy some of this — with the emphasis on the intern as the primary doctor for the patient (and then introducing the rest of the supporting team). But I think we can do more to change the culture and ensure that trainees continue to feel supported and valued in their role.