July 28th, 2022
10 Tips for July (and Beyond)
Madiha Khan, DO
For new trainees, starting July in the ICU can be the steepest of all learning curves, because the patient acuity and workflow can be overwhelming. The same is true for new fellows, I’ve found, as I started this month in the CCU. Although it is the same unit I worked in twice before as a resident, my new role encompasses more responsibility, contrasted with a more specialized focus in a highly complex subspecialty field. Working alongside the interns and trying to impart practical advice has offered me a unique perspective to be able to understand the gravity of both ends of the spectrum, while recognizing I still have a very long road ahead. In all honesty, these transitions, while an honor, are also hectic and ever changing and require adaptability on a moment-to-moment basis. Thankfully, I’ve learned a few key principles that have helped me pivot, adjust, and transition over this time — I still refer back to them.
1. Become comfortable being uncomfortable.
It’s no secret that the zone of growth occurs outside your comfort zone. I think we are actually better at this at the beginning of the transition period, where seemingly everything is foreign and uncomfortable. Inevitably, after getting the hang of a few things, it becomes harder not to cling onto familiar aspects and to continue to be in the growth mindset, and that’s when this reminder comes in handy most.
2. Work hard first, work smart later.
Being a new trainee, it feels like everyone above you can do your job, and can do it much quicker. Aside from streamlining the technical parts of the day (like reorganizing your EHR dashboard in a more efficient way), no hacks really shorten the process. Trying to do as much as possible yourself is cumbersome, but repetition and volume are the only ways to identify shortcuts without compromising the process.
3. Prioritize asking questions over having all the answers.
Remember to ask “why.” It’s good to have all the data points and lab values ready, but understanding the context in which they exist is crucial. It may seem like a win to finally identify and accurately present the worsening creatinine trend, but it is more important to ask why it is increasing.
4. Have the energy to learn.
What you put into training is what you get out of it. Every training program has a curriculum and didactics; however, being proactive in your own education allows you to address your own areas of weakness at your own pace.
5. Own your mistakes. Have a high tolerance for failure.
Everyone makes mistakes, but the way they handle making a mistake is what truly matters at the end of the day. Acknowledging the error is the crucial first step; only after owning the misstep can you truly be honest and clear about the thought process and identify areas for improvement.
6. Communication is key.
Breakdowns in communication are the breeding ground for mistakes and adverse events. Making sure everyone on the team is on the same page can be the most effective way to move things along in a hospital, and learning how to convey plans and ask questions clearly is a necessary skill to develop early.
7. Seek to simplify.
If you’re unable to explain a concept without overusing jargon, it may be an indication that you haven’t fully grasped it. Not to mention, shared decision making with patients is an important pillar of patient care that often falls short because of the clinician’s inability to simplify.
8. Embrace technology.
Are you having trouble keeping track of all your tasks? There is an app for that. Becoming comfortable with applications you use every day can save you hours of time in the future: from using templates for emails to utilizing a cloud-based server to access documents and educational materials across a variety of devices. Incorporating automation in your day-to-day routine can significantly improve your quality of life. (That being said, you don’t have to love every Epic update!)
9. Know when to say no.
No matter how many resiliency modules you complete, the compounded toll of being a trainee inevitably leads to some degree of burnout and exhaustion. Eating right, sleeping well, and working out seem to be the consistent advice to battle burnout — but equally important is to honestly assess your bandwidth to participate in extra curricular activities outside of training.
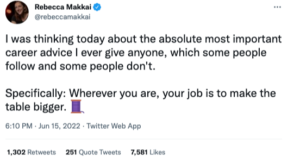
10. Make the table bigger.
Last but not least: root for others to succeed. There is enough success in the world for everyone. One of my favorite Twitter threads by author Rebecca Makkai outlines this idea beautifully. Even though she specifically talks about the arts, this idea absolutely applies to the world of academia.