August 29th, 2017
Procedures in Residency
Karmen Wielunski, DO

Karmen Wielunski, DO, is a 2017-18 Chief Resident in Internal Medicine at the Medical College of Wisconsin in Milwaukee
Hi. My name is Karmen, and I’m a fainter. It’s true. I am one of those people who occasionally falls victim (pun intended) to vasovagal syncope at its finest. It tends to happen at inopportune times and places. For example, the first time I passed out, I landed in a Christmas tree. I was in high school and suffering from a nasty viral illness, so I attributed the experience to volume depletion and moved on. However, shortly after starting clinical rotations in medical school, the Christmas tree incident came back to haunt me. Only this time, it was clear that clinical procedures were the culprit.
I quickly learned that some part of my brain has an aversion to blood – especially squirting blood – and it deals with this aversion by inducing syncopal events. This made for awkward experiences in operating and delivery rooms throughout medical school. It was frustrating, to say the least. People were understanding, but I still found myself avoiding certain situations in attempt to make as few “scenes” as possible.
Pre-Procedure Service Elective
When I started Internal Medicine residency, I was nervous. I knew my chosen career would keep me far away from operating rooms. But, I also knew I would be expected to learn how to perform certain procedures. In my mind, procedures meant blood, and blood meant syncope. I spent the first few months of my intern year contemplating how I was going to approach this issue. Eventually, I came up with the deeply insightful solution of “Maybe residency will be different!” So, I forged ahead.
Well, it turns out residency wasn’t different. The first sight of pulsating blood during my first arterial line attempt sent me straight to the floor. Luckily my senior was there to step in for me. I continued to attempt central and arterial lines during my months in the ICU, but I never felt confident. I knew I would always require someone with me for the times that my brain reminded me of its distaste for what I was doing.
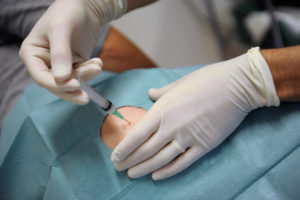
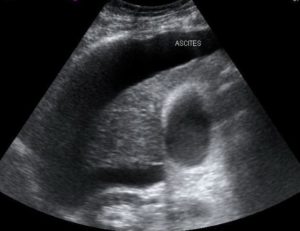
In a final effort to prove to myself that procedures simply didn’t suit me, I requested to rotate on our hospital’s procedure service elective. This is a service comprised of an attending and a resident who spend all day performing bedside procedures – mostly paracenteses, thoracenteses, and lumbar punctures. Residents love the rotation because the volume of procedures allows for excellent learning by repetition. It is also a great way to learn ultrasound skills, because all of the procedures are done with ultrasound guidance. Patients and various specialties also love this service because it is an avenue for these procedures to be done at the bedside in a timely manner.
Procedure Service Elective
On my first day on the service, we had 2 lumbar punctures planned for the morning. My attending said he would do the first one and go over every step with me and that I could try the next one. When we got started – I honed in on my osteopathic education and fairly easily located the appropriate disk spaces. My attending agreed with my findings and then showed me how to identify the intervertebral spaces and spinous processes with the ultrasound. He then went through each step of the lumbar puncture procedure. When he inserted the small needle into the patient’s back, a quick rush of panic came over me. “Please don’t faint, please don’t faint, please don’t faint.” Moments later, he pointed out the return of clear spinal fluid. I was intrigued, and I was still conscious! He systematically walked me through the remainder of the procedure. Before I knew it, we were moving onto the next patient. It was my turn.
As I greeted the next patient and started setting up, I focused on being as methodical as my attending. I appropriately positioned the patient, located the disk space and confirmed with ultrasound. With the kit open and sterile gloves on, I fumbled through opening the lidocaine and drawing it up. My attending systematically walked me through the steps, and before I knew it, I was ready. I advanced the lidocaine needle a little at a time, fully expecting to encounter bone and have to try again. But, the needle kept going, and I successfully anesthetized the patient on my first try. When it came time to advance the lumbar puncture needle, this also came more naturally to me than I expected. I slowly advance the needle and intermittently checked for clear fluid return. On the third check, there it was! Success! And, again, I was still conscious!
Post-Procedure Service Elective
By the end of the month-long rotation, I completed over 30 bedside procedures with zero syncopal events. I hadn’t really thought about the fact that not all procedures have a frequent squirting blood component; it turns out my brain has no aversion to clear-ish body fluids, and without the passing out component, I actually really enjoyed doing procedures. In 4 short weeks, I acquired a newfound confidence and a very useful set of skills. In retrospect, that was easily my favorite month of residency.
During the remainder of my time in residency, I experienced a sense of pride in my ability to perform these bedside procedures as well as teach other residents how to do them. This past week, during my first block as an attending physician, I was able to guide one of my interns through performing his first paracentesis using ultrasound guidance. He did very well. Afterwards, we discussed how empowering it is to be able to literally take the care of a patient into your own hands rather than relying on someone else to do it for you. I feel lucky to have trained at a place that houses such a great procedure service. It gave me confidence in an aspect of medicine that I didn’t think was possible for me. It also very much molded the way I will practice and teach medicine in the future.