May 2nd, 2014
A New Tool to Discuss Primary Prevention with a Statin with Patients: Life Expectancy Gain
Darrel P Francis, MD FRCP
A new Circulation study explores the spectrum of individual medication disutility for primary prevention of cardiovascular disease (CVD) in a sample of the general population, and juxtaposes it against the spectrum of expected longevity gain from initiation of statin therapy. Authors Darrel Francis, Professor of Cardiology at the National Heart and Lung Institute, Imperial College London, and Judith Finegold, Clinical PhD trainee in Cardiology, put the study’s findings into perspective for CardioExchange.
When we advise a patient on primary prevention of CVD we face a paradox. Current primary prevention practice recommends starting therapy largely based on cardiovascular risk. As age increases, annual risk goes up, which guideline convention interprets as increasing reason to initiate cardiovascular prevention (e.g., with statins). Taking this reasoning to its logical conclusion, however, initiation of statins would become mandatory in all of the very elderly. Practicing clinicians may feel uncomfortable with that concept.
There are two possibly unhelpful features of our current formal processes for deciding whether to recommend treatment with (for example) statins:
1. We judge the utility of initiating statin therapy, for life, based on artificially short time windows (e.g., 10 years), rather than examining lifetime benefit in terms of lifespan gain.
2. We assume that patients will universally consider prevention to be so desirable that it would always offset the inconvenience of having to take daily medication for life.
In our recently published study we present a new way of thinking about the pros and cons of cardiovascular primary prevention, and we propose two changes:
1. Estimate the benefit (utility) in terms of increase in life expectancy.
In our study we calculate not cardiovascular risk but life expectancy (i.e., lifespan) gain from a primary prevention intervention such as a statin (Figure 1). The pattern of life expectancy gain seems at first familiar, with increasing blood pressure and cholesterol associated with higher values (redder colors), but it has one crucial difference: Cardiovascular risk increases with increasing age, but life expectancy gain from statin initiation reduces with age of initiation. Initiating a lifetime of statins adds more to life expectancy if it is done earlier than later.
Figure 1. Distinction between cardiovascular risk and life expectancy gain. Both increase with increasing cholesterol and increasing blood pressure; but while risk (left panel) increases with age, the life expectancy gain from initiating a lifetime of preventative therapy (right panel) decreases with age. (The right panel is a simplified version of a chart in our paper, Fontana et al, Circulation 2014.)
2. Assess the patient’s willingness to take even an idealized medication to increase life expectancy: you might be surprised.
Population health policies have been based on the assumption that most people do not mind taking medication to increase their life expectancy, and, if patients do mind, this displeasure (called “disutility”) is so small as to be negligible compared to the financial cost of statins. However, with patent expiry, the financial cost of statins has fallen to near zero, so cost-effectiveness analyses can no longer afford to assume that disutility is zero or near-zero in everyone.
There are many reasons for not wanting to be on medication. We wanted to determine the lower limit on disutility in each subject, i.e., the disutility in an idealized situation where these main reasons are artificially removed. Real-world disutility is likely to be higher than that (but cannot be lower). We asked respondents to imagine a tablet treatment that had (a) no side effects, (b) no significant cost to them, (c) no requirement to visit a doctor, and (d) no consequences (apart from corresponding partial loss of benefit) of missing doses or stopping and restarting treatment at will.
Our study surveyed the general public. It found that, while there are many people who would be happy to take such an idealized medication for a small increase in life expectancy, there are also many who would do so only if the life expectancy increase was large. In fact, there is a substantial group who would not take daily medication even if it gave them 10 extra years of lifespan.
Figure 2. Juxtaposition of distribution of disutility (dislike of taking regular medication, upper panel) against distribution of utility (life expectancy gain from taking a statin, lower panel) in the general population. For patients with low disutility (green), regardless of their level of risk factors (and therefore utility) it appears rational to take preventative medication. For patients with high disutility (red), regardless of their level of risk factors, disutility seems to exceed utility. For the patients in between (the grey zone), the net effect of utility and disutility depends on their individual level of risk factors. Expressing both utility and disutility on a common scale, of extra life expectancy obtained or demanded, permits them to be juxtaposed easily and discussed openly. Redrawn from data in our paper, Fontana et al, Circulation 2014.
Our study indicates that there may be many patients whose dislike of daily medication may exceed the benefit delivered by statins. This becomes easy to see when both are expressed in common units such as lifespan gain.
It should be remembered that we have assessed only a lower limit on real-world disutility. We specifically asked respondents to assume there were no side effects. We did this to set aside the public controversy on whether statins do frequently cause side effects. A recent study from our group has examined the randomized blinded trial evidence on symptoms reported on statins versus on placebo, where both groups are given the same background information and same level of inquiry regarding symptoms. It found that under these blinded conditions there is very little difference between groups (i.e., very little incremental effect of statins). This information may at first seem difficult to believe when symptoms (such as muscle ache) are so common in daily primary prevention practice. However, the key message is not that the symptoms do not occur with statins, but rather that they occur equally on placebo when patients undergo the same level of questioning with neither the patient nor doctor knowing whether they are taking the real statin.
This calculation is not universally accepted because not everyone agrees that randomized, blinded, placebo-controlled data are the most reliable way to detect genuine mechanistic causation from other phenomena, as we have seen in the recent commotion over renal denervation . The powerful risk of bias from prior belief arising from our unblinded daily experience is all the more reason to seek out blinded data.
A new way to support primary prevention consultations?
Taken together, both our current and recent studies offer options for better-informed and more individualized consultations:
1. Doctors can now show patients charts that convey benefit of statin intervention in a readily understood language: that of life expectancy gain.
2. Doctors and patients now have reliable information on side effects, coming from 80,000 patients in blinded randomized controlled trials of statin versus placebo.
3. Patients can express their individual level of dislike of taking lifelong medication using the same metric (lifespan gain) as used to express
Ultimately, patients must make their own decisions and we must support them with the best quality information we can obtain.
Do you think the tools described here may be useful towards making primary prevention choices truly personalized?

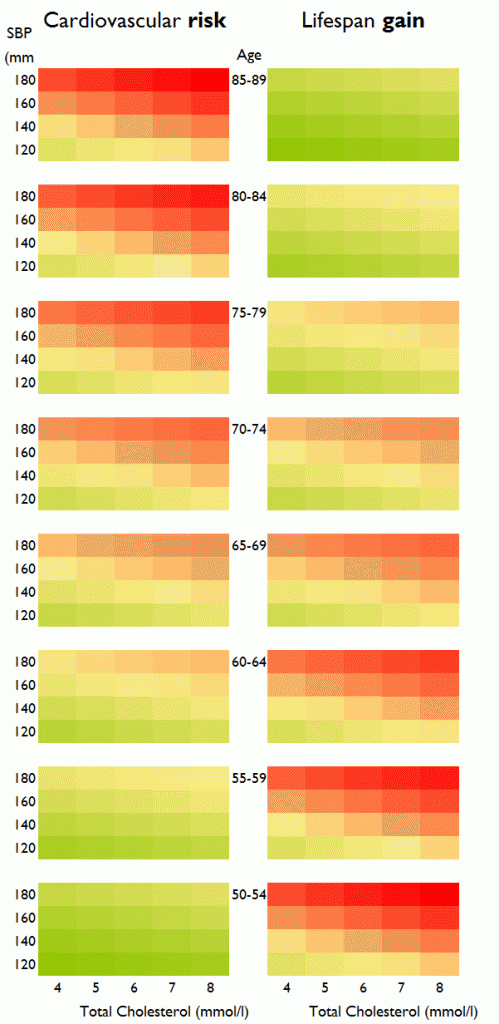
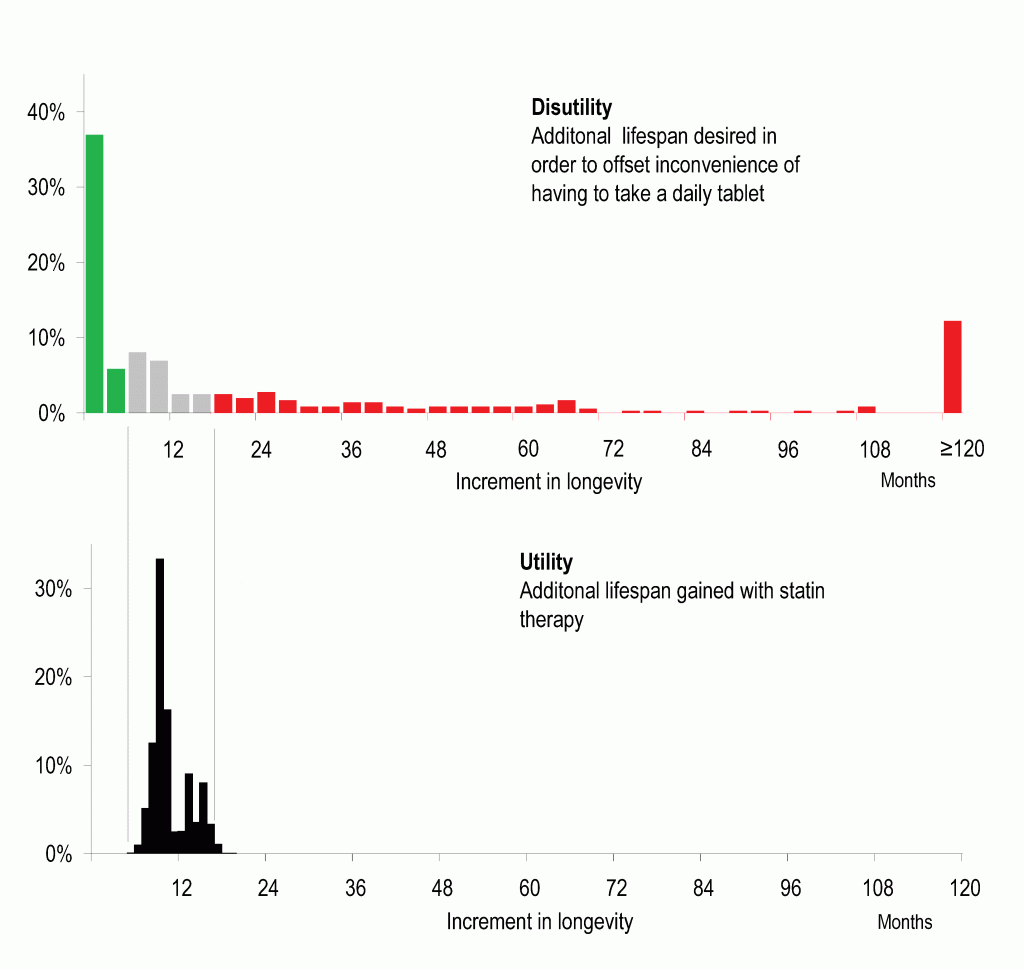
Figure 1 is an extraordinary visual conceptual display whose content is difficult to distill from any text/narrative. Now, I understand- finally. (You must be a student of Edward Tufte-author of “Beautiful Evidence’).
Is it to be understood from Figure 2 disutility graph that approximately 37% would take daily statin therapy FOR LIFE- to gain 3 months on longevity(first green bar)? Makes one circumspect of respondents understanding of the question(lifelong medication to gain 3 months of life vis a vis take medication in the next 3 months to prevent death within the next 3 months) or illustrates the very personalized value judgement- which , I believe is the point of disutility/utility reconciliation. If I interpret the concept and graph accurately, that 37% is as remarkable as the approximately 12% who expect 120 months of longevity to overcome their disutility. One would have expected the opposite proportionality.
Dear Dr Prida, Yes and Yes!
I am a huge fan of Tufte’s 3 books so it is a great honour to hear that the display brings his name to mind. The ingenuity of the juxtaposition between the right panel (from our paper) and the left panel, came from my clinical PhD trainee Judith Finegold.
And yes, 37% of people walking around on the streets of London would be happy to take a daily medication to give them an extra 3 months of life. Also there are 12% with extremely high disutility.
It should be remembered that they were asked to imagine an idealised agent that had (a) no side effects, (b) essentially no cost to them, (c) no doctor visits needed and (d) no obligation to take forever (i.e. preserved autonomy).
The paper originated from an afternoon when I asked Marianna Fontana to calculate the average lifespan gain from statin therapy, and she found it to be ~1-2 years. The immediate reaction from people in the room was “Bargain! If there is no hassle and no side effects, I would take it for even 2 or 3 months,” and contrastingly, “Not worth it! Why would I want to put artificial stuff in me for only 2 years extra?”.
The curious feature was not that each person had a different view. Rather it was that each person wrongly thought that everyone’s disutility would be closely clustered around his or her own personal value. The low-disutility and high-disutility people stared at each other in disbelief that they could unknowingly have been friends for years with people with such insane beliefs. That is when we decided to survey the general population. It turns out their spectrum was indeed wide.
The surprisingly wide distribution, and our individual inability as doctors to guess its shape, is the reason we should not make assumptions we know the answer for individual patients, when it is so simple to ask them.
Excellent statistical analisis and argumentation, without a doubt it is a tool to discuss primary prevention using statins.
As far as I know we use short time windows of 10 years, rather than examining lifetime benefit in terms of lifespan gain because we don’t have long follow up studies to predict risk for periods of time longer than 10 years. So this presentation assumes a great deal, trying to predict CV risk in the lifespan of our patients.
Doctors and patients now have reliable information on effects, coming from 80,000 patients in blinded randomized controlled trials of statin versus placebo but the longest follow up in the papers analyzed is 5.4 years and the average for all of them is much lower. So we don’t have reliable information on effects of the use of statins for long periods of time.
So the truth is we don’t now the effects and benefits using statins for very long periods of time and if they are going to increase the life span of our patients, specially in the low risk individuals
It would be more helpful and practical if they did a study balancing longevity benefits against healthier styles of life to discuss with our patients.
Thank you Dr Guadiana,
The story of why we use short horizons for calculations of risk is actually rather funny. A 2010 paper encapsulates it concisely:
In the covering editorial we couldn’t resist mischievously pointing out:
Regarding the 80,000 patients, I intended to say “side-effects” and I have asked Cardioexchange to insert the word “side-” to clarify.
Indeed we do not know the long term effects of statins. Trials have only maintained randomization for median times of up to ~5 years. Followup beyond this to ~11 years have consistently shown better outcomes in the statin arms. How we handle the uncertainty beyond this depends on which scenario we think more plausible:
(A) The statin effect on relative risk of cardiovascular events is broadly concordant across age groups, and therefore likely to be sustained lifelong. 10-year followup studies from RCTs show no sign of later net harm. Therefore our best estimate is that the effect of lifelong statins on relative risk of cardiovascular effects will be a simple extension of what is seen in the first few years. If so, our calculations in Circulation, which incorporate progressive increase in non-cardiovascular deaths with age, are reasonable.
(B) Alternatively, perhaps after a few years of statin treatment, the pathophysiology of atherosclerotic disease changes, so that continued statin use becomes incrementally harmful rather than beneficial. There is no sign of this happening in the trial data, so this would be conjecture. Under this hypothesis, our paper’s calculations would be incorrect.
Finally, I agree that it is always good to advise healthier lifestyles, even if the translation from words to action is more difficult than for tablet therapy. Sadly, RCTs addressing long-term mortality, which would be needed for our type of analysis, are scarce.
Thank you, Dr. Francis, for your answer, I admire your work. Without a doubt it is an excellent tool to discuss primary prevention with a Statin with patients. I see all the risk calculators as tools man made, so they are imperfect. Every intervention, like public health policies change the risk and explain much of the CVD decline in Western countries, so the risk analysis is in constant change.
In my experience many people desire better life span but many more are looking for quality of life so they don’t want to live longer if they are not going to have a good life, this could explain part of the discrepancies in your study.
I’m sure the phrase “Initiating a lifetime of statins adds more to life expectancy if it is done earlier than later” has its merits but at this moment it is a hypothesis since you already presented two scenarios, then we are waiting for the conclusion. So, it is an excellent tool, but at the same time we must be careful not to send a very good hypothesis as the truth. If you add to that phrase the word “it’s possible or even very possible” it would be 100% accurate.
One of the more difficult areas of medicine is prevention, to change the behavior of the population is a formidable task. The use of statins has increased exponentially in the last 15 years but at the same time caloric and fat intake have increased among statin users over time, which was not true for nonuser https://archinte.jamanetwork.com/data/Journals/INTEMED/0/ioi140043. We, the human race, are indeed difficult.
Regards,
Stranger than Paradise: Primary Prevention.
Nobody discuss and no one establishes Life span about High Blood Pressure (HBP) Treatment.
Do you only one second imagine a patient with HBP discussing the prescription (except side effects!)? Patients queue and interminably come to ask, to require, to impose upon us an antihypertensive treatment!
How many phone calls, unnecessary consultations have we because of this never-ending HBP and its supposed symptoms?
With hypercholesterolemia a crucial serial killer, if any, patients and our pairs disagree, discuss, compromise!
A contrario the example of HBP, discussion about the necessity and the goal of treatment of Hypercholesterolemia never ends!
Who can explain to me this discrepancy?
Who will be able to create a real marketing of hypercholesterolemia treatment in spite of indefinitely fuel the fear of Statins?
Like in Jim Jarmusch’s movie: It is Stranger than Paradise
Dear Dr. Francis,
It’s great to see you on CardioExchange!
I have a few quick thoughts, some of which I shared in the accompanying editorial (http://circ.ahajournals.org/content/early/2014/04/17/CIRCULATIONAHA.114.010152.short). First, although medication disutility can be measured, how to use it in clinical practice remains challenging, as there is considerable uncertainty for estimating risk and medication disutility at the individual level. (This is why, for example, we should be careful comparing the two panels of Figure 2 directly—it’s an apples and oranges comparison, as the top panel for disutility is comprised of individual measurements, but bottom panel is comprised of estimated statistical averages. One can easily imagine a 50 year old man in whom statins prevented a fatal MI, therefore gaining 25 years in longevity which would be off the horizontal axis for Figure 2; however this is a counterfactual that can never be measured directly, and regression-based methods would never yield an estimated longevity benefit that large.)
My overall feeling is that, for patients who are near the threshold for statin eligibility according the guidelines, disutility should play a larger role during the shared decision making process; for high risk patients, however, even if the expressed disutility is high, we need to try to understand the reasons for that disutility, to ensure that fears and concerns about statins are not “misfears”, to use the term Lisa Rosenbaum recently wrote about eloquently in a different clinical context (http://www.nejm.org/doi/full/10.1056/NEJMp1314638).
At a scientific level, I would also like to see more explorations of medication disutility and whether it is a fluid “trait” or a fixed “state” (or more likely a combination of the two). While working on the editorial, I was surprised to discover that the assumption of near-zero disutility for statins in the seminal cost-effective analyses were extrapolations from the disutility for aspirin and warfarin expressed by a-fib patients (http://archinte.jamanetwork.com/article.aspx?articleid=622371). These earlier studies were conducted in a more clinical context, and perhaps priming and context underlie some of the differences between these earlier studies and the present one. I would therefore be very interested to see future research assessing medication disutility in more clinical settings, such as during actual primary care visits, and using real medications including statins and anti-hypertensives instead of a theoretical tablet.
Finally, I would like to again congratulate you and your co-authors on your thought-provoking paper. Your story of how this research came about reminds me of how often we take for granted the simple assumptions we make in our daily clinical practice (such as most patients wouldn’t mind taking preventive medications). It’s great to see research examining these fundamental issues getting recognized!
Outstanding discussion.
With Dr. Francis’ repartee and Dr. Ye’s editorial extension(both which I have read more than once, now)the social context of scientific discourse of this blog- equating to being present in the same room questioning and listening to the thought “provocateurs”- should not be lost on our readership. Origins of research and ponderings not provided for in the refereed publication come to the fore.
Such rehashing brings clarity to the present science and serves as a platform for the knowledge gaps and lends insight to the next iterations.
Also, breaking out of the scientific self to be/think like a patient makes this a translatable exercise.
Thank you for the moment.
Dr. Francis. Congratulations of an impressive reconceptualization of medical decision making in primary prevention.
I do find it difficult, however, to understand how this information is helpful to patients. For patients to respond to a disutility survey, it would seem to me that they first have to believe that it is possible for a single intervention (pill) to add years (or months) to the lives of each person who takes it. As such, doesn’t this oblige us to discuss number needed to treat – acknowledging the fact that actually not everyone derives benefit.
Additionally, as Dr. Ye points out in his editorial, showing patients average life expectancy gain may obscure the point that some will die early (our traditional 10-year risk framework) at age 65, for example. Or that some patients will have an MI, but will not die – the trauma of an MI and possible sequelae of heart failure also needs to be acknowledged.
Assuming that we could accurately predict average life expectancy gain in the primary prevention setting, how do you propose we frame this for patients?
I agree with Erica. While I think that the concept of gain in life expectancy is very important for population health and cost-effectiveness analyses, I find it problematic as an approach to frame decision-making for an individual. When we talk about a life expectancy gain of 3 months for an individual, most patients would say that doesn’t sound like much. But of course, that isn’t how things work.
With any preventive intervention, some patients gain a year or 2, a rare few gain 5-10 years, and the vast majority gain nothing at all. This is embedded in the concept of risk and uncertainty that John Brush and others have attempted to depict, and is not at all evident from the average gain in life expectancy (which is truly only relevant to a large population).
This discussion is really interesting because it displays how hard it is to convey risk and probability to patients. Geniuses and polymaths have been arguing about the idea of probability for about 300 years. Yet, our patients come to a discussion of risk totally flat-footed. Very rarely do they come prepared to understand and talk about risk. Doctors need to help them, yet studies show that doctors often don’t understand risk either. Victor Montori’s tools are extremely useful for graphically displaying risk. I proposed a tool, the roulette wheel, that attempts to show that risk actually consists of two things: propensity (the design of the roulette wheel) and chance (the spin of the roulette wheel). Estimation of probability or risk for a single event or individual is a difficult notion. In my estimation, the thinking has to shift to a Bayesian notion of probability, which is a degree of belief or conviction. That degree of conviction, if properly estimated, will lead to a rational treatment plan.
I really enjoyed the discussion of disutility. It would be good to do a study of patient’s disutility related to anticoagulation. When I discuss the NOACs with patients, I find that the whole discussion is about trade-offs in disutility.
Very interesting discussion! I wonder how patients perceive utility or dis utility of other preventive approaches that are indeed devoid of side-effects, do not require doctors visits ( although such visits may be helpful), and are essentially free or their cost is expected to occur in a context of daily living. Specifically, I am referring to diet and exercise efforts in prevention. Would the utility and dis utility of these approaches be different from statins? How many years of life gained are afforded by being fit, and near- ideal waist circumference by decade of age? We are so focused on statins yet there is a much more powerful message to deliver, such as empowering patients in their own preventive efforts. Such efforts transform not just individuals, but entire families, and affect our younger generation. Moreover, in real world, the re is about 1 in 200 incidence of new onset diabetes with statins, as well as memory loss issues. These affect the very quality of life we are trying to prolong.
I still recall how early on in my training an established and wise clinician said we need to “treat patients to make them live longer, live better, or both”. However, if we cannot make them live better ( or at least convince ourselves that there is a certain degree of success in that), does living longer count? Can we as physicians offer our patients such a choice?
Dear Dr Druz
You make the excellent point that we have considered only artificial intervention with a table. Patients are already free to make diet and exercise modifications whenever they wish, which also does not require physician visits or monitoring and has no adverse events associated. We physicians are the barrier not to diet and exercise but to pharmaceutical intervention.
Certainly we should encourage healthy diet and exercise, but taking those steps too involve disutility which varies between individuals. While you and we and others on this blog may not find healthy eating and vigorous exercise aversive, there are others that do. In effect, these lifestyle interventions can be considered to have varying disutility, for example varying from strongly positive (for those who declare themselves allergic to gyms) through zero to negative (for those who enjoy exercise).
Isn’t it strange that as a society we fully accept people having such widely varying disutility for lifestyle interventions, but when it comes to taking medication our policies are built as though the disutility for everyone is the same and nearly zero?
Judith Finegold and Darrel Francis, London UK
I have a stupid courage to step in the conversation not reading the original article. Excuse me, please for this. Especially I am hesitating because my question is about the scales on the fig.1.
Left panel differentiates the ‘high’ and ‘low’ risk. The right panel pretends to show the time gain. But this gain may be represented in a different way.
E.g. all discussants presumed that it is the total time gained if one take the statin for the rest of life.
But, imagine that on the ordinate of the right panel will be not ‘time gained’, but time gained per one year of statin therapy. I believe, that the picture will change seriously. Probably, it will be like one on the left: the year of statin therapy started earlier will provide less added time of life.
Exposed to this information, I think, patients will want to delay the initiation of the therapy to have more ‘profitable deal’.
Dear Dr Vlassov,
Judith and I very much liked your deconstruction. Yes, lifespan gained per year would produce a pattern almost exactly like the left panel. This is because a short time horizon does not recognise that preventing a fatal event at the age of (say) 50 years permits many decades more of life, whereas preventing a fatal event at the age of 90 years is much less able to do so.
I can now use your argument to at last devise an invulnerable argument against Judith’s recommendation that I join a gym: although a year of participation may gain me some extra lifespan if I start now, the gain will definitely be larger if I start next year instead, and very much larger if I do it 10 years hence. With this logic I hope to ever remain a stranger to these weird voluntary workhouses, justifying my indolence with undeniable progressively increasing cost-effectiveness the longer I procrastinate.
By chance I have taken this question of progressively shorter analysis windows to its natural conclusion recently for statins. At the suggestion of the British Heart Foundation (http://tinyurl.com/BHF-statin-question) I have used the BHF’s Heart Protection Study and BHF national mortality statistics for Britain to calculate the death-prevention effect of statins on a daily (i.e. per-tablet) basis. Because the effect is small, I have put it into context with another death-prevention intervention in common use: the seatbelt.
As people age from the risk-seeking teenager to the cautious senior, the chance that wearing a seatbelt for a day will prevent death that day declines progressively. Meanwhile the chance that taking a statin for a day will prevent death rises progressively.
At some age, they curves will cross over. At what age do readers think this will happen?
Please guess, before checking at http://tinyurl.com/statin-versus-seatbelt
Probability and life expectancy are both group averages
Life expectancy is indeed an average, composed of adding up the individual lifespans of a group of people and dividing by the number of people. Probability, too, is an average. It is a series of “1”s for each person who has an event and “0”s for each who does not, added up, and divided by the number of people. Just as each person will have an individual lifespan which will certainly be different from the life expectancy, each person will have a different outcome which (being 1 or 0) will certainly be different from the probability. Nevertheless, if we can think about one type of group average, there is no reason we cannot think about the other.
Guidelines have established the habit of presenting one type of group average (probability) to the exclusion of the other (life expectancy). This has had two undesirable consequences.
First, guidelines assume patients’ attitude to prevention is uniform. If a recommendation is not to their liking they have no easy route to verbalise this, and instead are often labeled ‘non-compliant’ with medication
Second, focus on probability creates a perceived crescendo of need for primary prevention with progressive ageing. As physicians we all recognise that any calculation that leads to automatic blanket treatment of everyone at extreme high ages indicates there is a mistake in the approach. Perhaps we should take that realisation not as a special case, but as illuminating a problem with that guideline assumption that group-average risk (rather than group-average gain) should be the deciding factor.
Of course, as Drs Ye, Cohen and Spatz point out, averaging lifespan gain for an entire primary prevention population is a large over-simplification as the distribution of benefit is wide. However, we suggest that including possible life expectancy gain in a consultation may give physicians a way to express gain from a lifetime of intervention in a manner that may be readily comprehensible to many patients. Additionally it gives patients who are keen to take an intervention for even a small projected gain, a chance to exercise their wishes, which is a benefit both to the health of the nation and the principle of autonomy.
Judith Finegold and Darrel Francis, London UK