January 27th, 2012
Plaque Rupture with Thrombosis, After Shooting Hoops
Indu Poornima, MD and James Fang, MD
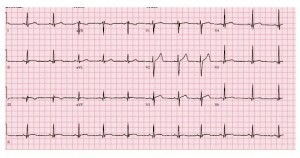
A 22-year-old white man presented to the ER with acute non-ST-segment-elevation MI, after playing basketball. He had experienced chest pain on and off for more than 10 hours before presentation. His initial EKG showed T-wave inversions in leads III and avF (see image), and his troponin T level was 1.2 ng/mL. The patient’s initial pain resolved with nitroglycerin, and he was transferred to a tertiary-care teaching hospital.
On arrival, he reported no pain but continued to exhibit the T-wave inversions in the inferior leads. Two-dimensional echocardiography, performed at bedside, showed normal wall motion and an LV ejection fraction of 55%. The patient was monitored in the CCU. He was started on aspirin and IV heparin.
One hour after admission the patient developed 18 beats of nonsustained ventricular tachycardia but remained asymptomatic. His troponin T level increased to 1.5 ng/mL, and he was taken to the catheterization lab, where he was found to have a proximal left-anterior descending plaque rupture with thrombus. He had distal TIMI 3 blood flow with an abrupt cutoff at the apical LAD that suggested an embolic process. Given the good distal flow, he was managed conservatively and started on prasugrel and integrilin, in addition to the heparin and aspirin. He was also given 80-mg atorvastatin (on admission, his LDL level was 76 mg/dL and his HDL level was 38 mg/dL). This regimen was continued for 2 days, during which the patient remained asymptomatic.
The patient was discharged on aspirin, prasugrel, and atorvastatin. His hypercoagulability workup was negative. He had no family history of premature coronary artery disease or sudden death, and no prior use of cocaine. However, he had recently started using supplements called Jack3d and Phenorex, which contain high doses of caffeine and a stimulant.
Questions:
1. Why would this healthy 22-year-old have developed plaque rupture and thrombosis?
2. What would be your long-term management strategy for this patient?
Response:
February 6, 2012
Myocardial infarction in people age 40 or younger has multiple etiologies, although accelerated atherosclerotic coronary artery disease remains the most common cause. This premature disease is often associated with lipid abnormalities such as familial hyperlipidemias and other lipoprotein disorders. For example, in Southeast Asian populations, abnormalities in lipoprotein(a) are common.
History alone is notoriously misleading in this clinical setting, so toxicology testing should be used to screen for use of cocaine, amphetamines, and other illicit drugs. Embolic disorders (e.g., myxoma and endocarditis) and coronary vasospasm should also be considered. Endothelial dysfunction could be addressed with brachial reactivity and/or ST-segment Holter monitoring for transient ST-segment elevation. I would not consider acetylcholine or ergonovine testing because of the potential risk during the peri-infarct period.
Other rare causes are divided into vasculopathies (e.g., vasculitis) and thrombophilias (e.g., antiphospholipid syndrome). Rarely, true connective tissue disorders (e.g., pseudoxanthoma elasticum) or metabolic disorders (e.g., involving homogentisic acid) may present with myocardial infarction.
In this case, it appears that most of these etiologies have been considered, although the specifics are not described. The use of supplements is notable and should be explored further.
I’d consider a coronary calcium score to assess whether a diffuse coronary vasculopathy is present, as well as a referral to a vascular medicine specialist to consider unusual vasculopathies.
The long-term management strategy should remain vigilant for the rare, potential etiologies described above, and the patient should continue to take aspirin and a statin. I would also consider the long-term use of dual antiplatelet therapy, despite the absence of any compelling data to support such an approach, because at his age the patient is at very low risk for bleeding.
Update:
February 13, 2012
The patient tested negative for other illicit drugs such as cocaine. His echocardiogram was negative for all other embolic causes. Erythrocyte sedimentation rate (ESR) was used to identify active vasculitis, and the result was negative. Specific testing for vasospasm was not planned, as this was not evident on the coronary angiogram. The plaque rupture was identified by the interventional cardiologist using intravascular ultrasound.
The patient has been seen in 3-week follow-up since hospital discharge. His workup included lipoprotein(a), ESR, gene mutations for prothrombin variants, antiphospholipid antibodies, and lupus anticoagulant — all were negative. Detailed lipoprotein analysis with a VAP test was normal.
The patient has been avoiding the use of supplements and continues to take aspirin, prasugrel, and atorvastatin. Follow-up echo continues to show normal LV function. He is scheduled for a symptom-limited stress test in 4 to 6 weeks, to determine whether he can return to sporting activities.
The plan is to continue dual antiplatelet therapy for 1 year, when the patient (who does not fall under any current guidelines) will be reevaluated. The appropriateness of high-dose atorvastatin in this setting is debatable, as several commenters here have noted. However, the fact that the patient’s initial event was plaque rupture, followed by acute thrombosis, led to this decision. He is also scheduled for a CT scan to detect coronary calcium, although I agree with Dr. Powell that the finding of an absence of calcification would not be very helpful in a 22-year-old.

1. Plaque at that age with lipids like that is strange. Hypercoag state is promoted with stimulants.
2. I’m not sure if he needs the lipitor. Its sounds like he may need some dietary counseling. Stay on ASA.
3. What were his TGs? If they were high it could mask hypercholesterolemia.
We all know that plaques form at a very early age but there is some inciting event that ruptures these plaques.
Most energy drinks contain stimulants. Red Bull (based on a thai drink) contains Lipovitan which is a mix of taurine, arginine etc. In most other energy drinks popular ingredients include caffiene in high doses, ginseng, herbs, various vitamins and things that no body knows. Some people mix them with alcohol and drink.
There have been case reports of acute coronary syndrome, arrhythmias, seizures and death after consumption of these energy shots. We had a similar case of a young male who presented with ACS after red Bull ingestion. A case of a 18 yr old basket ball player was reported too. A nice review on this topic is a refrence (Mayo Clin Proc. 2010 Nov;85 (11):1033-41.
I propose that a long term strategy for such patient is educating him about all this.
Anil Kumar
Cardiology department
Geisinger Medical Center
Competing interests pertaining specifically to this post, comment, or both:
none
Taurine and arginine are not stimulants. Taurine is antiarrythmic and arginine induces iNOS increasing nitric oxide production. Clearly stimulants (such as caffeine) could trigger a plaque rupture, however, as Dr. Kumar states. My question is how did such a young guy have plaque in the first place with such low LDL. My question remains what were his TGs?
My guess is he had hypertriglyceridemia.
There is obviously something here that we don’t understand, which I would think is rather the accentuation of the usual reality than an exception to it.
Thanks for all your input. The patient’s TG on admission was 66. We thought this was an unusual occurence too but managed him as we would any NSTEMI with the use of high-dose statin. I agree that the stimulants he was taking could have been responsible for triggering a plaque rupture and we did counsel him about discontinuing these supplements. Since he is only 22 the question is what other post-MI meds would you continue?
No atherectomy and stent placement?–even with good distal flow?
Competing interests pertaining specifically to this post, comment, or both:
No conflicts of interest.
just came across this news item in the NY times reporting 2 cases of AMI in the army after using Jack 3D-link attached.
http://www.nytimes.com/2012/02/03/business/army-studies-workout-supplements-after-2-deaths.html?
What about prinzmetals/spasm induced by the stimulants?
Competing interests pertaining specifically to this post, comment, or both:
none
Spasm and then thrombosis, both may relate to amphetamine-type agents. How do we know that there was a ruptured plaque? IV’US? Were the other coronary arteries angiographically pristine? Without evidence for underlying atherosclerosis, the stimulant takes the blame. The absence of coronary arterial calcification is not helpful in this age group. CTA for plaque may be helpful. If normal, gradual decrease and elimination of the “post-MI” drugs may be justified.
Autopsies done on soldiers killed in the Korean conflict of the early 1950’s showed what was then thought to be a surprising degree of atherosclerosis including coronary in such a Young population. Since a plaque has been demonstrated in him that probably had a soft cap that was affected by the stimulants, he should be kept on the statin. So far there are no long term negative side effects of that class. Is he an apoe 4 variant which I believe puts him at a higher risk for future events . His hdl is below 40 which also increases his long term risk. If he was 40c years old there would be only minimal discussion about the need for long term statin and other drugs. If he was 50 there would be no discussion. His diet also should be evaluated and modified for reducing the future risk of more Atherosclerosis.
Competing interests pertaining specifically to this post, comment, or both:
none
I agree with colleagues who preceded me in their conclusions. I would ask the presenters if they rule out VIH infection by viruses. One of the causes of coronary heart disease seen in young people without traditional cardiovascular risk factors is the presence of this condition.
answering dr. Brian Chou, MD prinzmetal angina is associated with transient ST segment elevation not st depression