February 17th, 2011
Quarter of U.S. Adults 45 and Older Taking Statins
Larry Husten, PHD
One-quarter of U.S. adults age 45 and older are taking statins, and one-half of men ages 65 to 74 are taking these drugs, according to the CDC’s annual report on trends in health statistics. From 1988 to 1994, only 2% of adults age 45 and older were taking statins. High cholesterol levels have been declining, according to the CDC, but hypertension, diabetes, and obesity have all increased. The overall prevalence of heart disease has remained stable in all groups except for an increased rate in men age 75 and older.
An article in Medpage Today includes comments from Christopher Cannon, James Stein, Robert Califf, and Harlan Krumholz.

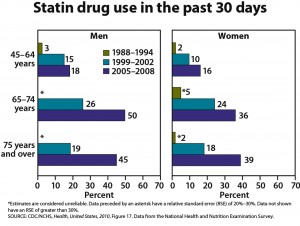
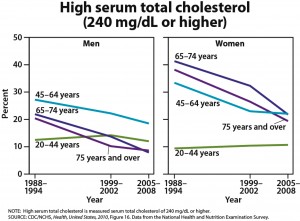
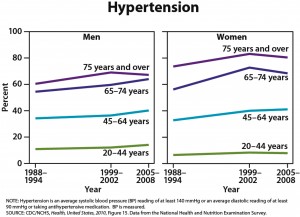
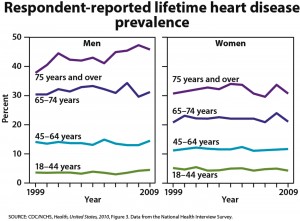
These statistics raise the important issue of unnecessary over-treatment–To the best of my knowledge, the “routine” use of statins has not been shown to reduce the incidence of death in people over age 75 years with hypercholesterolemia–Additionally, the prevalence of hypertension of~60-75 percent among people age 65 and older, a known risk factor for cardiovascular disease and death, raises the question of the frequency of anti-hypertensive therapy in these age groups, which is not addressed in this summary.
Competing interests pertaining specifically to this post, comment, or both:
None
The fact that heart disease kills more Americans than all cancers combined, it is not inappropriate that 1/4th of adults over 45 take statins. Over 1/4th of adults over 45 will die from CAD. Unfortunately, when we use conventional risk predictors, most individuals at highest risk for heart attacks are not being treated.
Sachdeva A et al. Am Heart J 2009; 157:111-117 found that only 14% of subjects presenting with their first MI were taking statin therapy. Considering that statins reduce MI by about 30% we must conclude that fewer than 25% of subjects at highest risk for MI are taking statins. Therefore, the inescapable conclusion is that the 25% of the population taking statins is not the 25% at risk for CAD.
If we could redirect the statins to those who truly need them and away from those with no potential for benefit, what a difference that would make. This is where atherosclerosis imaging excels and deserves further investigation and use.
Competing interests pertaining specifically to this post, comment, or both:
I use statins regularly, I treat patients with and without heart disease, I use EBT coronary calcium imaging and carotid ultrasound screening to distinguish who needs treatment and who does not. I saw no heart attacks in 2010.